मुख्य बातें
- Breast cancer is the most common cancer among women in the UAE, but 99% of early-stage cases are survivable with proper treatment — screening is what makes the difference
- Start annual mammograms at age 40 (or earlier with risk factors). 85% of breast cancers occur in women with NO family history, so every woman needs screening
- 3D tomosynthesis detects 20–40% more invasive cancers than standard 2D mammography and reduces false-positive callbacks by 15%, making it especially valuable for dense breasts
- The average mammogram pain score is 3.8 out of 10 — most women describe pressure, not pain. Compression lasts only 10–15 seconds per image
- BI-RADS categories 0–6 guide your next steps: 90–95% of abnormal mammograms turn out to be benign, so a callback does not mean cancer
- About 50% of women have dense breasts (Categories C–D), which both increases cancer risk and reduces mammogram sensitivity — supplemental ultrasound or MRI may be recommended
Let me share something that troubles me as a radiologist: I regularly diagnose breast cancer in women who "felt fine" and "had no symptoms." By the time cancer causes symptoms you can feel — a lump, skin changes, nipple discharge — it has already grown larger than we would like. The whole point of screening is to find cancer before you can feel it, when it is small and highly treatable.
Yet many women delay screening. Some are scared of what we might find. Others are busy with work and family. Some assume breast cancer only happens to women with family history (it doesn't — 85% of cases have no family history). Some had an uncomfortable mammogram years ago and never returned. Here is the reality: early-stage breast cancer has a 99% five-year survival rate. Advanced breast cancer has a much lower survival rate. Screening is what makes the difference. This guide explains everything — what a mammogram is, the different types, when to start, how to prepare, what the procedure involves, how to understand your results, what breast density means, and how mammograms compare with ultrasound and MRI.
What Is a Mammogram?
A mammogram (from the Latin mamma meaning breast and the Greek gramma meaning record) is a low-dose X-ray examination of the breast. It is the only imaging modality proven to reduce breast cancer mortality when used for routine screening, and it remains the gold standard recommended by every major medical organisation worldwide.
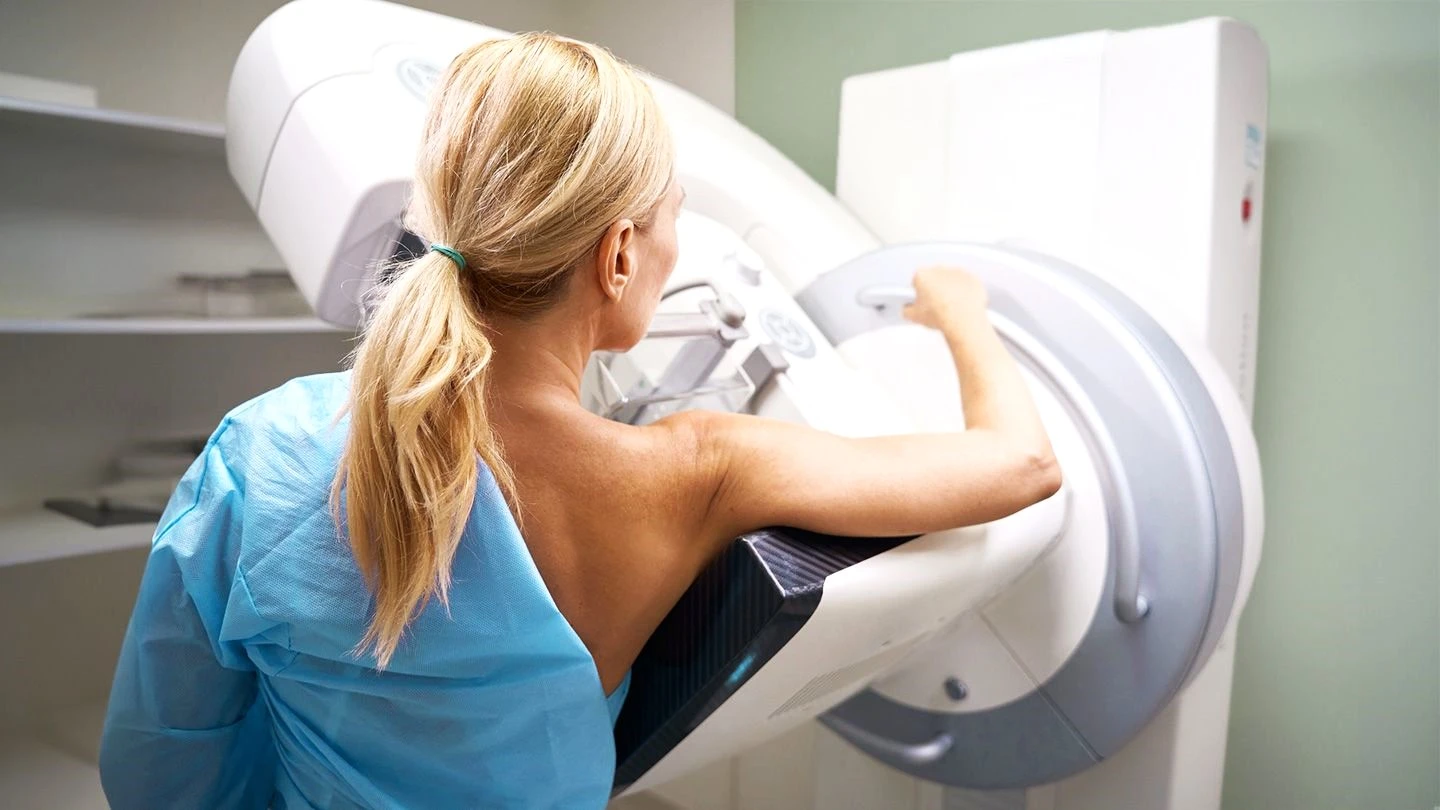
How Mammography Works
Each breast is positioned on a flat detector plate and gently compressed by a clear plastic paddle. The compression is essential — it spreads the tissue so we can see through all layers, reduces motion blur, improves contrast between different tissue types, and minimises the radiation dose required. We typically capture two images of each breast: a craniocaudal (CC) view taken from above, and a mediolateral oblique (MLO) view taken from an angle. The entire process takes about 15–20 minutes.
What Mammograms Detect
- Microcalcifications: Tiny calcium deposits that can indicate early cancer or pre-cancerous changes — often the earliest sign, detectable 1–3 years before a lump can be felt
- Masses: Solid or cystic lumps that may need further evaluation with ultrasound or biopsy
- Architectural distortion: Abnormal tissue patterns where breast tissue is pulled or distorted, which can indicate an underlying tumour
- Asymmetries: Areas that look different between the two breasts or compared with a previous mammogram
Mammogram Radiation Safety
A standard mammogram delivers approximately 0.4 mSv of radiation — equivalent to about 7 weeks of natural background radiation. To put this in perspective, a chest X-ray delivers 0.1 mSv and a transatlantic flight delivers 0.08 mSv. The cancer-detection benefit of regular mammography far outweighs this minimal radiation exposure, a fact confirmed by decades of research and endorsed by the FDA, WHO, and every major radiology society.
Types of Mammograms: 2D, 3D, Screening & Diagnostic
Not all mammograms are the same. Understanding the different types helps you make informed decisions about your breast health.
| Type | Description | Best For | Duration |
|---|---|---|---|
| Screening Mammogram | Routine exam for women with no symptoms. Standard 4 images (2 per breast). | Annual/biennial screening for women 40+ | 15–20 min |
| Diagnostic Mammogram | Targeted exam prompted by symptoms, abnormal screening result, or clinical concern. Includes additional views: spot compression, magnification, rolled views, exaggerated CC. | Evaluating lumps, pain, discharge, or prior abnormal findings | 30–45 min |
| 2D Digital (FFDM) | Standard full-field digital mammography. Captures flat 2D images of each breast from two angles. | Routine screening for average-density breasts | 15–20 min |
| 3D Tomosynthesis | X-ray tube sweeps in an arc (15–50°), capturing 9–25 low-dose exposures reconstructed into 40–80 thin slices at 1 mm thickness. | Dense breasts, high-risk women, reducing callbacks | 15–25 min |
Types of mammograms available in Dubai. Your radiologist will recommend the most appropriate type based on your breast density, risk factors, and clinical situation.
3D Tomosynthesis: The Evidence
3D mammography represents a significant advance over traditional 2D imaging. Instead of seeing all breast tissue compressed into a single flat image, the radiologist can scroll through the breast layer by layer — like slicing a loaf of bread and examining each slice individually. This eliminates the problem of overlapping tissue hiding cancers or creating false alarms.
The clinical evidence is compelling:
- JAMA Friedewald 2014 (454,850 exams): 41% more invasive cancers detected, 15% lower recall rate compared to 2D alone
- TOMMY Trial: Superior cancer detection in dense breast tissue specifically
- STORM Trial: 34% increase in overall cancer detection rate
- Malmö Trial: 38% increase in screen-detected cancers
Synthesised 2D (C-View by Hologic, V-Preview by GE) is a computer-generated 2D image created from the 3D data, eliminating the need for a separate 2D exposure. This keeps total radiation dose to approximately 1.5 mGy — well within the FDA maximum of 3.0 mGy per view.
2D vs 3D Mammogram: Key Differences
| Feature | 2D Digital Mammogram | 3D Tomosynthesis |
|---|---|---|
| Image Acquisition | 2 flat images per breast | 9–25 low-dose exposures reconstructed into thin slices |
| Cancer Detection Rate | Baseline | 20–41% higher (invasive cancers) |
| Callback Rate | Baseline (~10%) | 15% lower |
| Sensitivity in Dense Breasts | 48–64% | Significantly higher (exact varies by study) |
| Radiation Dose | ~1.2 mGy | ~1.5 mGy (with synthesised 2D) |
| Cost in Dubai (AED) | 250–500 | 500–900 |
| Best For | Average-density breasts, basic screening | Dense breasts, high-risk, reducing false positives |
2D vs 3D mammogram comparison. The cost difference is often offset by fewer false-positive callbacks that require expensive diagnostic workups.
For women with dense breasts or those who want the most thorough screening available, 3D tomosynthesis is worth the modest additional cost. A single avoided callback (with its diagnostic mammogram, ultrasound, and potential biopsy) can cost more than the price difference between 2D and 3D.
Breast Implants: Eklund Displacement Views
Women with breast implants can and should get mammograms. The technologist uses the Eklund displacement technique, gently pushing the implant back against the chest wall and pulling the natural breast tissue forward over it. This allows clear visualisation of the breast tissue in front of the implant. Additional images (typically 8 instead of 4) are taken to ensure complete coverage. Inform the scheduling staff about your implants when booking so extra time can be allocated.
When to Start Mammograms: Age & Risk Guide
Screening recommendations vary between organisations, but all agree on one principle: screening saves lives. The table below compares five major guidelines to help you and your doctor decide.
| Organisation | Risk Assessment | Age 40–44 | Age 45–54 | Age 55–74 | Age 75+ |
|---|---|---|---|---|---|
| American Cancer Society (ACS) | By age 25 | Optional annual | Annual | Biennial (or annual) | Continue if 10+ yr life expectancy |
| USPSTF (2024 Update) | — | Biennial | Biennial | Biennial (to 74) | Insufficient evidence |
| American College of Radiology (ACR) | By age 25 | Annual | Annual | Annual | Continue if 10+ yr life expectancy |
| UAE DHA / SEHA | — | Annual | Annual | Biennial (50–69) | Shared decision |
| WHO | — | Annual if resources permit | — | Biennial (50–69) | — |
Major breast cancer screening guideline comparison (2024–2026). The USPSTF updated its recommendation in 2024 to start biennial screening at 40 instead of the previous 50.
UAE-Specific Context
These global guidelines are particularly important for women in the UAE because the average age at breast cancer diagnosis in the UAE is approximately 49 — over a decade younger than the average in the US and Europe (approximately 62). Furthermore, 23% of breast cancer diagnoses in the UAE occur in women under 40, and a higher percentage of women present at advanced stages compared with Western populations. This underscores why starting screening at 40 (or earlier for high-risk women) is especially critical in our region.
Risk Factor Assessment
Your personal risk level determines when and how often you should be screened. Here is an important fact: 75–85% of breast cancers occur in women with NO family history. Having no risk factors does not mean you are safe — it means you are at average risk, and you still need regular screening. Discuss your personal risk profile during your annual women's health consultation to ensure your screening plan is appropriate.
| Risk Factor | Risk Multiplier | Screening Implication |
|---|---|---|
| First-degree relative with breast cancer | 2–4× average risk | Start screening 10 years before their diagnosis age |
| BRCA1 mutation | 45–65% lifetime risk | Annual MRI from age 25 + mammogram from 30 |
| BRCA2 mutation | 45–72% lifetime risk | Annual MRI from age 25 + mammogram from 30 |
| Dense breasts (Category D) | 4–6× average risk | Annual mammogram + supplemental ultrasound or MRI |
| Prior chest radiation (age 10–30) | 3–5× average risk | Annual MRI + mammogram starting 8 years after radiation |
| Personal history of breast cancer | 3–4× average risk | Annual mammogram + possible MRI |
| Atypical ductal hyperplasia | 4–5× average risk | Annual mammogram, consider MRI |
| Lobular carcinoma in situ (LCIS) | 7–12× average risk | Annual mammogram + MRI |
| Hormone replacement therapy (combined) | 1.2–1.7× average risk | Annual mammogram while on HRT and for 5 years after |
Breast cancer risk factors and their screening implications. Risk models such as Tyrer-Cuzick, Gail Model, and BRCAPRO help calculate your individualised lifetime risk.
Screening by Age Group
Age 20–39 (Average Risk): Formal mammographic screening is not routinely recommended. Focus on breast awareness (knowing your normal) and clinical breast exams every 1–3 years. If you have high-risk factors — BRCA mutation, chest radiation between ages 10–30, Li-Fraumeni or Cowden syndrome, first-degree relative with premenopausal breast cancer, or ≥20% lifetime risk on validated models — screening with MRI (and possibly mammography) should begin as early as age 25.
Age 40–49: This is where the annual vs biennial debate lives. A modelling study published in Cancer found 40% more breast cancer deaths when biennial screening started at 50 compared with annual screening from 40. Given the younger average age of breast cancer diagnosis in the UAE, we recommend annual screening from age 40.
Age 50–74: All guidelines agree that screening in this age range saves lives. Evidence shows a 25–30% reduction in breast cancer mortality, preventing 8–21 deaths per 1,000 women screened over 10 years. Annual or biennial frequency depends on your individual risk profile.
Age 75+: Screening decisions should be based on overall health and life expectancy. If you have more than 10 years of life expectancy and are in good health, continuing screening is recommended. If life expectancy is 5–10 years, it becomes a shared decision with your doctor. Screening may reasonably stop when life expectancy is under 5 years.
How to Prepare for a Mammogram
Proper preparation ensures the clearest images and the most comfortable experience. Follow these evidence-based tips.
When to Schedule
If you are still menstruating, schedule your mammogram during the follicular phase (days 7–10 after the start of your period). This is when oestrogen and progesterone levels are lowest, and breast tissue is least tender, least swollen, and easiest to compress comfortably. Avoid scheduling during the week before your period when breasts are most sensitive.
Products to Avoid (and Why)
On the day of your mammogram, do not apply any of the following products to your chest, underarms, or breasts:
| Product | Why It Must Be Avoided |
|---|---|
| Deodorant / Antiperspirant | Contains aluminium particles that appear as white specks on the mammogram, mimicking microcalcifications — the earliest sign of breast cancer |
| Body Powder / Talc | Metallic particles create artifacts that can obscure real findings |
| Body Lotion / Cream | May contain metallic compounds (zinc, titanium) that create imaging artifacts |
| Perfume | Some formulations contain metallic particles |
| Sunscreen | Zinc oxide and titanium dioxide (common UV filters) appear as calcifications on images |
Products to avoid before a mammogram. Shower normally but skip all products from the waist up on the morning of your appointment.
Day-of Checklist
- Morning routine: Shower without applying any products to your chest or underarms. Remove all jewellery (necklaces, chains, body piercings)
- Getting dressed: Wear a two-piece outfit so you only undress from the waist up. Skip underwire bras (they must be removed and create marks on images)
- What to bring: Emirates ID or passport, insurance card, list of current medications, any prior mammogram images or CDs from other facilities, a list of breast concerns or symptoms to discuss
- Caffeine: Consider reducing caffeine intake for 1–2 days before your appointment if you have fibrocystic breasts — caffeine can increase breast tenderness
- Pain management: If you are particularly sensitive, take 400 mg ibuprofen 30–60 minutes before your appointment
Breastfeeding and Pregnancy
You can get a mammogram while breastfeeding. Nurse or pump immediately before your appointment to reduce breast fullness, which improves image quality and comfort. The radiation dose does not affect breast milk. During pregnancy, mammography is considered safe if clinically indicated (the radiation dose to the foetus is negligible with abdominal shielding), though diagnostic ultrasound is the preferred first-line imaging tool during pregnancy.
Do I Need a Referral in Dubai?
Many imaging centres in Dubai, including DCDC, accept self-referrals for screening mammograms. You do not need a doctor's referral to book a routine screening appointment. However, insurance coverage may require a referral for reimbursement — check with your provider.
What Happens During a Mammogram: Step-by-Step
Knowing what to expect eliminates anxiety. Here is exactly what happens from the moment you arrive.
| Step | What Happens | Duration |
|---|---|---|
| 1. Check-in & Gown | You change into a gown from the waist up. A female technologist explains the procedure and confirms your history. | 5 minutes |
| 2. Positioning | The technologist positions one breast on the detector plate and adjusts your arm and shoulder for optimal tissue coverage. | 2–3 min per view |
| 3. Compression | The clear paddle lowers to compress your breast firmly but briefly. You may feel pressure or discomfort — this is normal and necessary. | 10–15 sec per view |
| 4. Image Capture | The X-ray exposure fires. You must hold still and may be asked to hold your breath briefly. | <1 sec per exposure |
| 5. Additional Views (if needed) | For diagnostic mammograms: spot compression, magnification, rolled views, or exaggerated CC views may be taken. | 5–10 min |
| 6. Review & Dressing | The technologist reviews images for technical quality. If adequate, you dress and the images go to the radiologist for interpretation. | 5 minutes |
Standard mammogram procedure timeline. A screening mammogram involves 4 images (2 per breast). A diagnostic mammogram may involve 8 or more images.
Screening vs Diagnostic Mammogram
| Feature | Screening Mammogram | Diagnostic Mammogram |
|---|---|---|
| Purpose | Routine check for women with no symptoms | Investigating symptoms, abnormal findings, or follow-up |
| Who Orders | Self-referral or GP | Referring physician or radiologist |
| Standard Views | 4 (CC + MLO, both breasts) | 4 standard + additional targeted views |
| Additional Techniques | None | Spot compression, magnification, rolled views, tomosynthesis |
| Duration | 15–20 minutes | 30–45 minutes |
| Radiologist Present | Images reviewed after appointment | Often reviewed in real-time, may add views during exam |
| Results Timeline | 1–2 weeks (standard), same-day available | Often same-day or within 24 hours |
| Cost (AED) | 250–700 | 400–900 |
Screening vs diagnostic mammogram comparison. If your screening mammogram shows something that needs further evaluation, you will be called back for a diagnostic mammogram.
Does a Mammogram Hurt? Pain & Comfort Guide
Pain is the number one reason women delay or avoid mammograms. Let me share what the research actually shows — and practical strategies to minimise discomfort.
What the Research Says
A meta-analysis of over 200,000 women found that 90% reported some discomfort during mammography, but only 11% described it as "painful." The average pain score is 3.8 on a 10-point scale — firmly in the "uncomfortable but tolerable" range. Compression lasts only 10–15 seconds per image, and the entire exam involves about 60 seconds of total compression time.
| Pain Score (0–10) | Description | Percentage of Women |
|---|---|---|
| 0–2 | Minimal — slight pressure, easily tolerable | 25–30% |
| 3–5 | Moderate — noticeable pressure, compare to a firm blood-pressure cuff | 50–55% |
| 6–7 | Significant — uncomfortable but brief | 15–20% |
| 8–10 | Severe — uncommon, may indicate underlying issue | <5% |
Mammogram pain distribution (meta-analysis, n = 200,000+). Mean pain score: 3.8/10.
Why Compression Is Necessary
- Tissue separation: Spreads overlapping tissue so abnormalities are visible rather than hidden behind other structures
- Reduced radiation: Thinner tissue requires a lower dose to produce a clear image
- Improved contrast: Uniform thickness creates consistent image quality across the entire breast
- Reduced motion blur: Immobilised tissue produces sharper images
Factors That Affect Comfort
- Menstrual cycle phase: Breasts are most tender in the luteal phase (week before period). Schedule during the follicular phase (days 7–10 after period start)
- Breast density: Denser breasts may require firmer compression and can be slightly more uncomfortable
- Caffeine intake: Caffeine can increase breast tenderness in some women, particularly those with fibrocystic changes
- Anxiety level: Tension causes muscles to tighten, which increases perceived discomfort. Relaxation techniques help significantly
- Breast size: Both very small and very large breasts can present positioning challenges that affect comfort
- Previous surgery or implants: Scar tissue or implants may alter sensation during compression
7 Proven Tips to Reduce Discomfort
| Tip | When | How It Helps |
|---|---|---|
| Schedule during follicular phase | When booking | Breasts are least tender (lowest hormone levels) |
| Reduce caffeine 1–2 days before | 48 hours prior | Decreases breast tissue sensitivity |
| Take 400 mg ibuprofen | 30–60 min before | Reduces inflammation and pain perception |
| Practice relaxation breathing | During compression | Slow deep breaths reduce muscle tension and anxiety |
| Communicate with the technologist | During exam | She can adjust positioning and compression speed for comfort |
| Request a comfort pad | At appointment | Foam pads placed on the compression plate cushion the breast |
| Apply a cool compress after | Post-exam | Reduces any residual tenderness |
7 evidence-based tips for a more comfortable mammogram experience.
When Pain Is Abnormal
While brief discomfort during compression is normal, the following are not typical and should be reported:
- Severe bruising that lasts more than a few days
- Persistent pain lasting more than 48 hours after the exam
- New skin changes (redness, swelling, dimpling) after the exam
- A new palpable lump that was not present before
- Fever or signs of infection
Is a 3D mammogram more painful than 2D? No. The compression is similar for both. Some women actually report slightly less compression with 3D because the technology can produce diagnostic-quality images with marginally less force.
Understanding Your Mammogram Results: BI-RADS Explained
Every mammogram report includes a BI-RADS (Breast Imaging Reporting and Data System) category, a standardised system developed by the American College of Radiology that tells you and your doctor exactly what was found and what should happen next. Understanding these categories eliminates the anxiety of waiting for results.
| BI-RADS | Category | What It Means | Cancer Risk | Next Steps |
|---|---|---|---|---|
| 0 | Incomplete | More imaging needed — the mammogram was not sufficient for a final assessment | Unknown until resolved | Additional mammogram views, ultrasound, or prior images for comparison |
| 1 | Negative | Completely normal mammogram. No masses, calcifications, or asymmetries. | Essentially 0% | Routine screening in 1–2 years |
| 2 | Benign | A finding that is definitively benign — such as cysts, calcified fibroadenomas, fat-containing lesions, or implants | 0% | Routine screening in 1–2 years |
| 3 | Probably Benign | A finding with <2% chance of malignancy. Typically a non-palpable, well-defined mass or focal asymmetry | <2% | Short-interval follow-up: 6, 12, 18, and 24 months |
| 4 | Suspicious | A finding that does not have the classic appearance of cancer but is abnormal enough to warrant tissue sampling | 2–95% (4a: 2–10%, 4b: 10–50%, 4c: 50–95%) | Biopsy recommended |
| 5 | Highly Suggestive of Malignancy | A finding with classic cancer appearance — spiculated mass, pleomorphic calcifications, or suspicious enhancement | >95% | Biopsy required; treatment planning begins |
| 6 | Known Biopsy-Proven Malignancy | Cancer has already been confirmed by biopsy. This category is used for imaging during treatment planning. | Confirmed | Surgical planning, staging, treatment |
BI-RADS categories 0–6. The vast majority of screening mammograms are BI-RADS 1 (negative) or BI-RADS 2 (benign finding).
Being Called Back: What It Really Means
About 10% of women are called back after a screening mammogram for additional imaging (BI-RADS 0). Before you panic, understand this: 90–95% of callbacks result in a benign finding. Only about 1 in 10 callbacks (approximately 1% of all screened women) will ultimately be diagnosed with cancer.
The six most common reasons for callbacks are:
- Overlapping tissue: Normal tissue layers created a suspicious-looking shadow that needs to be resolved with additional views
- Dense breast tissue: Dense tissue can obscure or mimic abnormalities, requiring ultrasound to clarify
- Technical issues: Motion blur, positioning artifacts, or incomplete coverage that require repeat images
- New finding: Something not seen on prior mammograms that needs characterisation
- No prior comparison: First mammogram at a facility, so the radiologist cannot compare with previous images
- Architectural distortion: A subtle change in tissue pattern that needs additional evaluation
BI-RADS 3 Follow-Up Protocol
If your finding is categorised as BI-RADS 3 (probably benign), you will follow a structured surveillance protocol: imaging at 6 months, then 12 months, then 18 months, then 24 months. If the finding remains stable throughout this period, it is downgraded to BI-RADS 2 (benign) and you return to routine screening. The rationale is that cancers grow and change, while benign findings remain stable.
If Biopsy Is Recommended
A biopsy sounds frightening, but it is usually a straightforward, minimally invasive procedure. The most common type is a core needle biopsy, performed under local anaesthesia using ultrasound guidance. A small needle extracts several tissue samples for microscopic analysis. The procedure takes about 30 minutes, leaves no significant scarring, and you can return to normal activities the same day. Results are typically available within 2–5 business days.
How long do mammogram results take? Screening mammogram results are typically available within 1–2 weeks. For diagnostic mammograms, results are often available same-day or within 24 hours. At DCDC, we prioritise rapid reporting because we understand that waiting for results causes significant anxiety.
Patient Experience: Sarah's Callback Story
"I received the call that my screening mammogram showed something and I needed to come back. I was terrified — I didn't sleep for two nights. When I came back for the diagnostic mammogram and ultrasound, Dr. Elzamzami explained everything in real-time. It turned out to be overlapping tissue that looked suspicious on the screening image. My final result was BI-RADS 2 — completely benign. I cried with relief. The callback was scary, but I'm so grateful the system works the way it does. I'd rather have a thorough check that causes a brief scare than miss something real." — Sarah, 46, Dubai
Breast Density: What It Means for Your Screening
Breast density is one of the most important factors in mammographic screening, yet most women have never heard of it. Your breast density is determined by the ratio of fibroglandular tissue (which appears white on a mammogram) to fatty tissue (which appears dark). You cannot feel breast density — it can only be assessed on imaging.
| Category | Description | Prevalence | Cancer Risk | Mammogram Sensitivity |
|---|---|---|---|---|
| A: Almost Entirely Fatty | Breasts are almost entirely composed of fat | 10% of women | Baseline | Highest (>90%) |
| B: Scattered Fibroglandular | Scattered areas of density, but mostly fatty | 40% of women | Baseline | Good (80–90%) |
| C: Heterogeneously Dense | Many areas of density that may obscure small masses | 40% of women | 1.2–2.1× baseline | Reduced (65–80%) |
| D: Extremely Dense | Nearly the entire breast is dense tissue | 10% of women | 4–6× baseline | Lowest (48–64%) |
ACR breast density categories. Approximately 50% of women have dense breasts (Categories C or D). Density is assessed from your mammogram and reported to you.
The Masking Effect
Dense breast tissue appears white on a mammogram. Cancers also appear white. This creates a "masking effect" — like trying to find a snowball in a snowstorm. In extremely dense breasts (Category D), mammogram sensitivity drops from the typical 85–90% to as low as 48–64%. This means that roughly 1 in 3 cancers may be missed by mammography alone in very dense breasts. The callback rate is also twice as high for dense breasts because overlapping tissue creates more suspicious-looking shadows.
Supplemental Screening for Dense Breasts
If you have dense breasts, your radiologist may recommend additional screening beyond mammography:
- Breast Ultrasound: The ACRIN 6666 trial showed that supplemental ultrasound detects 2–4 additional cancers per 1,000 women with dense breasts that mammography alone missed. The trade-off is a higher false-positive rate (PPV 8.9%), meaning more women will be called back for findings that turn out to be benign
- Breast MRI: The most sensitive option with 95% sensitivity in dense breasts, but expensive (AED 3,000–6,000), time-consuming (30–60 minutes), requires contrast injection, and has even higher false-positive rates. Recommended for women with dense breasts plus high-risk factors
- Contrast-Enhanced Mammography (CEM): A newer technique that combines standard mammography with an iodine-based contrast injection. It achieves sensitivity approaching MRI while using the familiar mammography workflow and at a lower cost. Available at select centres in Dubai
Who Should Get Additional Screening?
- Women with Category D (extremely dense) breasts on mammography
- Women with Category C (heterogeneously dense) breasts plus additional risk factors
- Women with strong family history plus dense breast tissue
- Women with a personal history of breast cancer plus dense breasts
Does Breast Density Change Over Time?
Yes. Breast density typically decreases with age, particularly after menopause, as glandular tissue is gradually replaced by fatty tissue. Weight gain can also decrease density. Conversely, hormone replacement therapy can increase breast density, which is one reason HRT use warrants closer screening. About 60–70% of breast density is genetically determined — if your mother had dense breasts, you are more likely to as well.
Mammogram vs Breast Ultrasound vs Breast MRI
These three imaging modalities each have distinct strengths and limitations. They are complementary tools — not replacements for each other.
| Feature | Mammogram | Breast Ultrasound | Breast MRI |
|---|---|---|---|
| Technology | Low-dose X-rays (FFDM or tomosynthesis) | High-frequency sound waves (7–18 MHz transducer) | Magnetic fields + radio waves + gadolinium contrast |
| Radiation | Yes (0.4 mSv — minimal) | None | None |
| Sensitivity (Overall) | 85–90% | 80–85% (operator-dependent) | 94–99% |
| Sensitivity (Dense Breasts) | 48–64% | 80–85% | 77–94% |
| Specificity | 88–95% | Lower (PPV 8.9% in ACRIN 6666) | 72–85% (more false positives) |
| Detects Calcifications | Excellent — primary method | Poor — cannot reliably detect microcalcifications | Limited |
| Detects Soft-Tissue Masses | Good | Excellent — distinguishes solid from cystic | Excellent |
| Duration | 15–20 min | 15–30 min | 30–60 min |
| Contrast Required | No | No | Yes (gadolinium IV injection) |
| Cost (AED) | 250–900 | 400–600 | 3,000–6,000 |
| Best For | Routine screening (gold standard) | Evaluating lumps, dense breast supplement, pregnancy, young women, biopsy guidance | BRCA carriers, very high-risk, staging known cancer, implant integrity |
Mammogram vs breast ultrasound vs breast MRI comparison. No single modality is perfect — the optimal approach combines tools based on your individual risk profile and breast characteristics.
Can Ultrasound Replace Mammography?
No. While ultrasound is excellent for evaluating palpable lumps and supplementing mammography in dense breasts, it cannot replace mammography for routine screening. The key limitation: ultrasound cannot reliably detect microcalcifications, which are often the earliest and only sign of breast cancer or pre-cancerous changes. Additionally, the ACRIN 6666 trial showed that ultrasound screening has a positive predictive value (PPV) of only 8.9% compared with mammography's 25–40%, meaning far more false positives. Ultrasound complements mammography; it does not replace it.
When to Choose Ultrasound
- Evaluating a palpable lump: Ultrasound excels at distinguishing solid masses from fluid-filled cysts. A simple cyst is almost always benign and often needs no treatment
- Supplemental dense breast screening: Added to mammography for Category C or D breasts
- Pregnancy or lactation: No radiation — safe first-line imaging during pregnancy. Nurse or pump before the exam for better image quality
- Women under 30: Primary imaging tool for younger women (dense tissue makes mammograms less useful, and younger tissue is more radiation-sensitive)
- Biopsy guidance: Real-time imaging allows precise needle placement for core biopsies and aspirations
When to Choose MRI
- Known BRCA1/BRCA2 mutation carriers: Annual MRI starting at age 25–30, alternating with mammography on a 6-month rotation (mammogram month 1, MRI month 7, mammogram month 13, and so on)
- ≥20% lifetime risk based on validated risk models (Tyrer-Cuzick, BRCAPRO)
- First-degree relative of BRCA carrier who has not been tested themselves
- Chest radiation between ages 10–30 (e.g., Hodgkin lymphoma treatment)
- Li-Fraumeni, Cowden, or Bannayan-Riley-Ruvalcaba syndrome
- Staging known breast cancer: Evaluating extent of disease before surgery
- Monitoring treatment response: Assessing tumour shrinkage during chemotherapy
- Implant integrity: Checking for silicone implant rupture (MRI is the gold standard)
- Occult primary: When cancer is found in axillary lymph nodes but mammogram and ultrasound cannot locate the breast source
MRI limitations: MRI is not recommended for average-risk screening because its lower specificity (72–85%) leads to more false positives and unnecessary biopsies. It also cannot reliably detect calcifications, requires IV gadolinium contrast (which carries rare risks in patients with kidney disease), and takes 30–60 minutes in a confined space (claustrophobia can be an issue).
Patient Experience: Nadia's Alternating Schedule
"I tested positive for a BRCA2 mutation after my mother was diagnosed with breast cancer at 52. Dr. Elzamzami set me up on an alternating schedule — mammogram every January, breast MRI every July. It means I'm checked every six months with a different modality. At 38, my MRI detected a tiny lesion that the mammogram from six months earlier had not shown. It was caught at stage IA — the earliest possible stage. The alternating schedule quite literally may have saved my life." — Nadia, 38, Dubai
Patient Experience: Amira's Breastfeeding Scare
"I found a lump while breastfeeding my second baby. I panicked. My doctor sent me for a breast ultrasound first because I was lactating. The ultrasound showed it was a galactocele — basically a milk-filled cyst that had blocked. No cancer, no biopsy needed, just follow-up in three months. The ultrasound was painless and gave me my answer in minutes. If the ultrasound had been unclear, I would have been sent for a mammogram next, but it resolved everything." — Amira, 35, Abu Dhabi
Special Situations
Young Women (Under 30)
Routine mammographic screening is not recommended for women under 30 because breast tissue in younger women is typically very dense (reducing mammogram effectiveness), younger tissue is more sensitive to radiation, and breast cancer in this age group is uncommon. If a young woman presents with a breast concern, ultrasound is the first-line imaging tool. However, for high-risk young women (BRCA carriers, prior chest radiation, strong family history), MRI screening may begin as early as age 25.
Post-Treatment Surveillance
Women who have been treated for breast cancer require ongoing surveillance mammography. Guidelines typically recommend annual mammography of the treated breast (if breast-conserving surgery was performed) and the opposite breast. MRI may be added if there are additional risk factors. The first post-treatment mammogram is usually performed 6–12 months after completing radiation therapy.
Baseline Mammogram
The ACR recommends that women get a baseline mammogram between ages 35 and 40. This baseline image serves as a comparison point for future screening mammograms, making it easier to detect subtle changes over time. If you are over 40 and have never had a mammogram, there is no need for a separate baseline — your first screening mammogram becomes your baseline.
Breast Self-Exam: What the Evidence Says
The role of breast self-examination (BSE) in cancer screening has shifted significantly over the past two decades. While formal monthly self-exams are no longer universally recommended as a screening tool, breast self-awareness — knowing how your breasts normally look and feel — remains valuable and is endorsed by every major medical organisation.
Why Formal Monthly Self-Exams Are No Longer Recommended
Two large randomised controlled trials (Shanghai 2002, n=266,064 and Russia 2003, n=120,310) found that formal monthly BSE did not reduce breast cancer mortality and led to a significant increase in benign biopsies — meaning more women underwent invasive procedures for findings that were not cancer. Based on this evidence, the USPSTF, WHO, and Canadian Task Force all recommend against teaching formal monthly BSE as a screening strategy.
Breast Self-Awareness: What You Should Do Instead
Rather than a rigid monthly routine, experts recommend breast self-awareness — an ongoing familiarity with how your breasts normally look and feel at different times of the month. This allows you to notice changes promptly and report them to your doctor.
Changes to Report to Your Doctor Immediately
- New lump or thickening: Any hard, painless mass or area that feels different from the surrounding tissue — especially if it does not change with your menstrual cycle
- Skin changes: Dimpling, puckering, redness, or an orange-peel texture (peau d'orange) on any part of the breast
- Nipple changes: Inversion (nipple pulling inward) that is new, persistent discharge (especially bloody or clear), or scaling/flaking of the nipple skin
- Size or shape changes: One breast becoming noticeably different in size or shape compared with the other
- Persistent pain: Localised pain in one specific area that does not go away after your period (most breast pain is hormonal and bilateral — not cancer)
- Swelling: Swelling in or around the breast, collarbone area, or armpit without an obvious cause
Important: Self-awareness complements but does not replace professional screening with mammography. Many breast cancers are too small to feel — screening mammograms detect cancers 1–3 years before they become palpable. The combination of breast self-awareness plus regular mammography provides the most comprehensive approach to early detection.
BRCA Gene Testing and Genetic Counselling in Dubai
BRCA1 and BRCA2 are tumour suppressor genes that help repair DNA damage. When either gene carries a harmful mutation, the body's ability to fix DNA errors is compromised, dramatically increasing the risk of breast and ovarian cancer. Understanding your BRCA status can be life-changing — it allows you and your doctor to implement enhanced screening and risk-reduction strategies that can catch cancer at its earliest, most treatable stage or prevent it entirely.
BRCA1 vs BRCA2: The Numbers
| Risk Factor | General Population | BRCA1 Mutation | BRCA2 Mutation |
|---|---|---|---|
| Lifetime breast cancer risk | 12% (1 in 8) | 55–72% | 45–69% |
| Breast cancer before age 50 | ~2% | 30–40% | 20–30% |
| Ovarian cancer risk | 1.2% | 39–44% | 11–17% |
| Second breast cancer (contralateral) | ~5% over 10 years | 40–60% lifetime | 26–40% lifetime |
| Male breast cancer | 0.1% | 1–5% | 5–10% |
BRCA mutation cancer risk compared to general population. Source: National Cancer Institute, SEER data.
Who Should Consider BRCA Testing?
BRCA testing is not recommended for the general population. It is most informative for individuals with specific risk indicators:
- Family history: Two or more first-degree relatives (mother, sister, daughter) with breast cancer, or one relative diagnosed before age 50
- Ovarian cancer: Any first-degree relative with ovarian cancer at any age
- Male breast cancer: A male relative with breast cancer
- Bilateral breast cancer: A relative with cancer in both breasts
- Ashkenazi Jewish heritage: Higher prevalence of BRCA1/2 founder mutations (1 in 40 vs 1 in 300–500 in general population)
- Triple-negative breast cancer: Diagnosed under age 60
- Known family mutation: A relative who has tested positive for BRCA1/2
- Multiple cancers: Breast and ovarian cancer in the same individual or family
What Happens If You Test Positive?
A positive BRCA result does not mean you will definitely develop cancer — it means your risk is significantly elevated. Your medical team will discuss a comprehensive risk-management plan:
- Enhanced screening: Annual breast MRI starting at age 25–30 alternating with mammography every 6 months, creating a surveillance schedule that checks you twice a year with different modalities
- Risk-reducing medications: Tamoxifen or raloxifene can reduce breast cancer risk by 30–50% in high-risk women
- Prophylactic surgery: Bilateral mastectomy reduces breast cancer risk by 90–95%. Bilateral salpingo-oophorectomy (removal of ovaries and fallopian tubes) reduces ovarian cancer risk by 80–90% and breast cancer risk by ~50% when performed before menopause
- Lifestyle optimisation: Regular exercise, healthy weight maintenance, limited alcohol, and breastfeeding (if applicable) all modestly reduce risk even in BRCA carriers
BRCA and Genetic Testing Cost in Dubai
| Test Type | Cost Range (AED) | What It Covers |
|---|---|---|
| BRCA1/BRCA2 panel | AED 2,500 – 4,500 | Tests for known pathogenic mutations in BRCA1 and BRCA2 genes |
| Multi-gene panel (20–80 genes) | AED 4,000 – 8,000 | BRCA1/2 plus additional cancer risk genes (PALB2, ATM, CHEK2, TP53, etc.) |
| Genetic counselling session | AED 500 – 1,000 | Pre-test risk assessment and post-test results interpretation with a certified genetic counsellor |
| Family member targeted test | AED 800 – 1,500 | Tests a specific known family mutation in a relative |
Genetic testing costs in Dubai (2026). Some insurance plans cover BRCA testing for women who meet NCCN high-risk criteria.
Genetic counselling is strongly recommended both before and after BRCA testing. A trained genetic counsellor assesses your family history, explains what the results mean, helps you understand your options, and provides emotional support. Testing without counselling can lead to misinterpretation and unnecessary anxiety. BRCA and other genetic tests are processed through our laboratory services, and for genetic counselling and testing referrals in Dubai, speak to your physician at DCDC's Gynecology & Obstetrics department.
Breast Cancer Screening Cost in Dubai: Complete Comparison
Understanding the cost of different screening options helps you plan your breast health strategy. Here is a complete comparison of breast cancer screening costs in Dubai for 2026:
| Screening Method | Cost Range (AED) | Who Needs It | Frequency |
|---|---|---|---|
| 2D Digital Mammogram | 250 – 500 | All women 40+ | Annual or biennial |
| 3D Tomosynthesis Mammogram | 500 – 900 | Dense breasts, high-risk, first-timers | Annual |
| Breast Ultrasound | 400 – 600 | Dense breasts (supplemental), lumps, women under 30 | As recommended |
| Breast MRI | 3,000 – 6,000 | BRCA carriers, ≥20% lifetime risk, prior chest radiation | Annual (alternating with mammogram) |
| BRCA Genetic Test | 2,500 – 4,500 | Strong family history, specific risk criteria | Once (lifetime result) |
| Clinical Breast Exam | 200 – 400 | Part of annual checkup for all women | Annual |
| Comprehensive Screening Package | 500 – 1,200 | Mammogram + ultrasound + consultation | Annual |
Breast cancer screening costs in Dubai (2026). Most insurance plans cover annual screening mammograms for women 40+ as preventive care. For detailed mammogram pricing, see our <a href="/blog/mammogram-cost-dubai" class="text-primary-600 hover:underline">mammogram cost guide</a>.
The cost of screening is a fraction of the cost of treating advanced breast cancer. Late-stage treatment can exceed AED 200,000–500,000+ including surgery, chemotherapy, radiation, and ongoing medication. A 20-minute mammogram at AED 250–900 is one of the highest-value investments in your health.
Know Your Risk — Book a Breast Health Assessment
Not sure which screening you need? Our specialists can assess your risk profile and recommend the right screening plan for your age, breast density, and family history. Contact DCDC to schedule your assessment.
Breast Screening at DCDC Dubai Healthcare City
At our Dubai Healthcare City clinic, we provide comprehensive breast imaging services designed for accuracy, comfort, and efficiency:
- Digital mammography and 3D tomosynthesis with experienced female technologists trained in comfort-first positioning techniques
- Breast ultrasound for lump evaluation, dense breast supplemental screening, and biopsy guidance
- Same-day supplemental ultrasound: If your mammogram reveals dense breasts or a finding requiring further evaluation, we can perform ultrasound immediately — no separate appointment needed
- Ultrasound-guided core needle biopsy when tissue sampling is needed, with results typically in 2–5 business days
- Rapid reporting: Diagnostic mammogram results often available same-day. Screening results within 24–48 hours
- Walk-in and self-referral welcome: No doctor's referral required for screening mammograms
- Insurance accepted: We work with all major UAE insurers. Most policies cover annual screening mammograms for women 40+ as preventive care
- Coordination with breast surgeons and oncologists if treatment is required — seamless referral pathway
Book Your Mammogram Today
Early detection is within your control. Regular screening finds cancer when it is most treatable — and a 99% survival rate speaks for itself. At Doctors Clinic Diagnostic Center in Dubai Healthcare City, our experienced radiologists provide comprehensive breast imaging including mammography, breast ultrasound, and biopsy services. Whether you are due for your annual screening or have a concern that needs evaluation, we are here to help.
DCDC में संबंधित सेवाएं
दुबई हेल्थकेयर सिटी में विशेषज्ञ देखभाल और उन्नत निदान
अक्सर पूछे जाने वाले प्रश्न
Take Control of Your Breast Health
Early detection is the most powerful weapon against breast cancer. When found early, the five-year survival rate is 99%. When found late, it drops dramatically. Screening is what bridges that gap — and the 15–20 minutes a mammogram takes is a small investment for such a significant return.
Whether you are booking your first mammogram at 40, managing dense breasts with supplemental imaging, or following up on a finding with your radiologist — you are taking control of your health. Do not let fear, misconceptions about who gets breast cancer, or a busy schedule delay your screening. Book your breast screening at our Dubai Healthcare City clinic today. For cost information, see our mammogram pricing guide.
स्रोत एवं संदर्भ
यह लेख हमारी चिकित्सा टीम द्वारा समीक्षित है और निम्नलिखित स्रोतों का संदर्भ देता है:
- American Cancer Society — Breast Cancer Screening Guidelines (2024)
- USPSTF — Updated Breast Cancer Screening Recommendations (2024)
- American College of Radiology — Breast Imaging Recommendations
- JAMA — Friedewald et al. (2014): Breast Cancer Screening Using Tomosynthesis (n=454,850)
- ACRIN 6666 Trial — Supplemental Screening Ultrasound for Dense Breasts
- Journal of the National Cancer Institute (JNCI) — Breast Density and Cancer Risk
- Dubai Health Authority (DHA) — Breast Cancer Screening Programme
- RadiologyInfo.org — Mammography Patient Information
- WHO — Breast Cancer Early Detection and Screening
- TOMMY Trial & STORM Trial — Tomosynthesis Clinical Evidence
इस साइट पर चिकित्सा सामग्री DHA-लाइसेंस प्राप्त चिकित्सकों द्वारा समीक्षित है। हमारी देखें संपादकीय नीति अधिक जानकारी के लिए।
Related Articles

Mammogram Cost in Dubai: Prices, Insurance & Free Options (2026)
10 Early Signs of Breast Cancer Every Woman Should Know
Women's Health Screening Guide
Cancer Screening in Dubai: Tests, Costs & What to Expect
blogPage.moreFromCategory

Pregnancy Scan Schedule Dubai: Trimester Guide (2026)
और पढ़ें
PCOS Treatment Dubai: Diagnosis & Care (2026)
और पढ़ें
HPV Test Dubai: Types, Cost & Screening (2026)
और पढ़ें
NT Scan Dubai: Cost, Timing & Results (2026)
और पढ़ें
Pregnancy After HSG Test Dubai: Success Rates (2026)
और पढ़ें
NIPT vs Amniocentesis: Which Test to Choose (2026)
और पढ़ें© 2026 Doctors Clinic Diagnostic Center (DCDC), Dubai Healthcare City. Originally published at https://doctorsclinicdubai.ae/blog/breast-cancer-screening-guide. All rights reserved. Unauthorized reproduction is prohibited.