Key Takeaways
- Breast cancer is the most common cancer in women worldwide, and early detection through screening increases the five-year survival rate to over 99% when caught at stage I
- The 10 early warning signs include a new lump, skin dimpling, nipple discharge, nipple retraction, skin texture changes, swelling, persistent breast pain, redness or warmth, changes in breast size or shape, and swollen lymph nodes under the arm
- Women aged 40 and older should have an annual mammogram; women aged 20 to 39 should perform monthly self-examinations and have a clinical breast exam every one to three years
- Mammography remains the gold standard for breast cancer screening, while ultrasound is an essential complementary tool for women with dense breast tissue
- DCDC in Dubai Healthcare City offers comprehensive breast screening services including digital mammography and breast ultrasound with same-day results from experienced radiology specialists
Breast cancer is the most frequently diagnosed cancer among women globally, accounting for approximately 2.3 million new cases each year according to the World Health Organization. In the United Arab Emirates, breast cancer represents the leading cancer diagnosis in women, making awareness of early warning signs and consistent screening a matter of critical importance. The single most powerful factor in breast cancer survival is early detection: when breast cancer is identified at stage I, the five-year survival rate exceeds 99%, compared to approximately 30% when diagnosed at stage IV. This stark difference underscores why every woman should know the early signs of breast cancer, understand the screening options available, and take proactive steps to protect her health.
This comprehensive guide covers the 10 early warning signs of breast cancer that every woman should recognize, explains when to see a doctor immediately, reviews the key risk factors, compares mammogram and ultrasound screening methods, outlines age-specific screening guidelines, provides a step-by-step self-examination guide, and details where to access breast cancer screening at Doctors Clinic Diagnostic Center (DCDC) in Dubai Healthcare City.
10 Early Warning Signs of Breast Cancer
Breast cancer does not always present with obvious symptoms in its earliest stages, which is precisely why routine screening is so important. However, there are specific physical changes that can serve as early warning signals. Recognizing these signs of breast cancer and acting on them promptly can be the difference between an early-stage diagnosis with excellent outcomes and a late-stage diagnosis with significantly reduced survival rates. The following are the 10 early signs that every woman should be aware of.
1. A New Lump or Mass in the Breast
The most common and widely recognized sign of breast cancer is a new lump or mass in the breast. Cancerous lumps are often hard, irregularly shaped, and painless, though some may be soft, round, or tender. A lump that feels distinctly different from the surrounding breast tissue, that persists throughout the menstrual cycle, or that appears to be growing warrants immediate medical evaluation. It is important to note that not all lumps are cancerous, as many are benign cysts or fibroadenomas, but only a medical professional can make that determination through appropriate imaging and, if necessary, biopsy.
2. Skin Dimpling or Puckering
When a tumor grows beneath the skin and pulls on the connective tissue (Cooper's ligaments) that supports the breast, it can create visible dimpling or puckering on the skin surface, sometimes resembling the texture of an orange peel. This phenomenon, known medically as peau d'orange, is a significant warning sign that should never be ignored. Skin dimpling can appear on any part of the breast and may be subtle initially, becoming more pronounced as the underlying tumor grows.
3. Nipple Discharge (Especially Bloody or Clear)
Nipple discharge that occurs spontaneously (without squeezing), affects only one breast, and is bloody, clear, or straw-colored can be an early indicator of breast cancer or a precancerous condition such as ductal carcinoma in situ (DCIS). While many causes of nipple discharge are benign, including hormonal changes, infections, and benign papillomas, any spontaneous unilateral discharge should be evaluated by a physician with appropriate imaging studies.
4. Nipple Retraction or Inversion
A nipple that suddenly turns inward (retracts) when it previously projected outward is a concerning sign. Nipple retraction occurs when a tumor located behind the nipple pulls the nipple tissue inward as it grows. Some women naturally have inverted nipples from birth, which is not a cause for concern. However, a new change in nipple direction, particularly on one side only, requires prompt medical attention.
5. Skin Texture Changes
Changes in the texture of the breast skin, including thickening, roughness, scaliness, or a rash-like appearance, can indicate breast cancer. Paget's disease of the nipple, a rare form of breast cancer, presents as a red, scaly, crusty rash on the nipple and areola that may be mistaken for eczema or dermatitis. If a skin change on the breast does not respond to standard dermatological treatments within a few weeks, breast cancer should be investigated as a possible cause.
6. Unexplained Swelling of the Breast
Swelling of part or all of the breast, even without a distinct lump, can be a sign of inflammatory breast cancer (IBC), an aggressive form that accounts for 1 to 5 percent of all breast cancers. IBC causes the breast to appear swollen, red, and warm because cancer cells block the lymphatic vessels in the skin. This type of breast cancer can develop rapidly over days to weeks and is often initially mistaken for an infection. Any sudden, unexplained increase in breast size should be evaluated without delay.
7. Persistent Breast Pain in One Area
While breast cancer is typically painless in its early stages, persistent pain that is localized to one specific area of the breast and does not fluctuate with the menstrual cycle can sometimes be an early symptom. Breast pain (mastalgia) is extremely common and is most often related to hormonal changes, caffeine intake, or musculoskeletal causes. However, pain that is unilateral, constant, progressively worsening, and accompanied by any other changes on this list should be investigated.
8. Redness or Warmth of the Breast Skin
Redness, warmth, or a purple discoloration of the breast skin that does not resolve with antibiotics is another hallmark sign of inflammatory breast cancer. The affected breast may feel noticeably warmer than the other breast. Because these symptoms closely mimic those of a breast infection (mastitis), IBC is frequently misdiagnosed initially. If antibiotic treatment for a suspected breast infection fails to produce improvement within seven to ten days, further investigation with imaging and possible biopsy is essential.
9. Change in Breast Size or Shape
A noticeable change in the size or shape of one breast compared to the other, particularly if the change develops over a short period, can indicate an underlying tumor. While slight asymmetry between the two breasts is normal and common, a new or progressive difference in size, contour, or hang should be brought to medical attention. This is especially significant when accompanied by skin changes, a visible mass, or distortion of the breast profile when the arms are raised above the head.
10. Swollen Lymph Nodes Under the Arm or Near the Collarbone
Breast cancer can spread to the axillary (underarm) lymph nodes even before the primary tumor in the breast is large enough to be felt. A hard, painless, or fixed lump in the armpit or above the collarbone that persists for more than two weeks and is not associated with an obvious infection or recent vaccination may indicate that breast cancer cells have reached the regional lymph nodes. Swollen lymph nodes in these locations should always be evaluated with imaging and, if appropriate, biopsy.
"The most important message I give to women is that early breast cancer often has no symptoms at all, which is exactly why regular screening is so essential," says Dr. Osama Elzamzami, Head of Radiology at DCDC. "But when symptoms do appear, acting on them within days rather than weeks or months can dramatically change the outcome."
When to See a Doctor Immediately
While many breast changes turn out to be benign, certain signs require urgent medical evaluation. You should see a doctor as soon as possible if you experience any of the following:
- A new breast lump or thickening that persists for more than one menstrual cycle or is present in postmenopausal women
- Bloody or clear spontaneous nipple discharge from one breast
- Rapid onset of breast swelling, redness, and warmth that does not respond to antibiotics within 7 to 10 days
- Visible skin dimpling, puckering, or peau d'orange (orange peel appearance) on the breast
- A new nipple retraction or inversion that was not previously present
- A hard, fixed lump in the armpit that persists for more than two weeks
- Any combination of two or more warning signs appearing simultaneously
Do not wait for a scheduled screening appointment if you notice any of these changes. Early evaluation with clinical examination and appropriate imaging, typically a mammogram and ultrasound, is the first step toward ruling out or confirming breast cancer and initiating treatment as quickly as possible. Your internal medicine physician can coordinate referrals for imaging and specialist consultations.
Breast Cancer Risk Factors
Understanding your personal risk factors for breast cancer helps you make informed decisions about how frequently to screen and what lifestyle modifications may reduce your risk. Risk factors fall into two categories: those you cannot change (non-modifiable) and those you can influence (modifiable). For related information, see our guide on Breast Cancer Screening: Mammogram & BRCA Guide.
Non-Modifiable Risk Factors
- Gender: Being female is the single greatest risk factor. Men can develop breast cancer, but it is approximately 100 times more common in women
- Age: The risk of breast cancer increases with age. Approximately 80% of breast cancers are diagnosed in women over the age of 50
- Family history: Having a first-degree relative (mother, sister, or daughter) with breast cancer approximately doubles your risk. The risk increases further if the relative was diagnosed before the age of 50 or if multiple family members are affected
- Genetic mutations: Inherited mutations in the BRCA1 and BRCA2 genes significantly increase lifetime breast cancer risk to 45-72%, compared to approximately 13% in the general female population. Blood tests including BRCA genetic screening can help identify carriers of these mutations
- Personal history: Women who have had breast cancer in one breast have a three to four times higher risk of developing a new cancer in the other breast or a different part of the same breast
- Dense breast tissue: Women with dense breast tissue (more glandular and connective tissue relative to fatty tissue) have a 1.5 to 2 times higher risk of breast cancer and their tumors are harder to detect on mammograms
- Early menstruation or late menopause: Starting periods before age 12 or entering menopause after age 55 increases lifetime estrogen exposure, which is associated with a modestly increased risk
Modifiable Risk Factors
- Physical inactivity: Regular physical activity (at least 150 minutes per week of moderate exercise) is associated with a 20-25% reduction in breast cancer risk
- Alcohol consumption: Even moderate alcohol intake increases breast cancer risk. Women who consume two to three drinks per day have approximately 20% higher risk than non-drinkers
- Obesity after menopause: Excess body fat after menopause increases estrogen production, which is linked to higher breast cancer risk. Maintaining a healthy BMI is protective
- Hormone replacement therapy (HRT): Combined estrogen-progesterone HRT used for more than five years increases breast cancer risk. The risk decreases after discontinuation
- Not breastfeeding: Breastfeeding for a cumulative total of one year or more over a lifetime is associated with a modest reduction in breast cancer risk
"Having risk factors does not mean you will develop breast cancer, and many women diagnosed with breast cancer have no identifiable risk factors beyond being female and aging," says Dr. Osama Elzamzami, Head of Radiology at DCDC. "This is why screening is recommended for all women, regardless of their perceived risk level."
How Breast Cancer Is Detected Early
Early detection of breast cancer relies on a combination of self-awareness, clinical examination, and imaging-based screening. Each method plays a distinct role in identifying breast cancer at its most treatable stage. Women should discuss their individual risk factors with their gynecologist and consider comprehensive cancer screening that addresses breast, cervical, and other gynecological cancers together. The three pillars of early detection are:
- Breast self-examination (BSE): A monthly self-check that helps women become familiar with the normal look and feel of their breasts, enabling them to recognize changes early
- Clinical breast examination (CBE): A physical examination performed by a trained healthcare professional who systematically palpates the breast tissue, nipple, and axillary lymph nodes to check for abnormalities
- Imaging-based screening: Mammography (the gold standard), breast ultrasound, and breast MRI, which can detect cancers that are too small to feel during a physical examination
Screening mammography is the only imaging method that has been proven in large randomized controlled trials to reduce breast cancer mortality. The landmark studies conducted since the 1960s have consistently demonstrated that regular mammographic screening reduces breast cancer deaths by 20 to 40% in women aged 40 to 74. This mortality reduction is achieved because mammography can identify tumors as small as 2 to 3 millimeters, often years before they would become palpable.
Book Your Breast Cancer Screening
At Doctors Clinic Diagnostic Center in Dubai Healthcare City, our radiology team provides comprehensive breast cancer screening including digital mammography and breast ultrasound. Get accurate results with same-day reporting from experienced radiology specialists.
Mammogram vs Ultrasound for Breast Screening
Two primary imaging modalities are used in breast cancer screening: mammography and ultrasound. Each has distinct strengths and limitations, and in many cases, both are used together for the most comprehensive evaluation. Understanding the differences helps women appreciate why their doctor may recommend one or both methods.
Mammography uses low-dose X-rays to create detailed images of the internal breast tissue. It is the gold standard for breast cancer screening because it is the only imaging method proven to reduce breast cancer mortality in clinical trials. Mammography excels at detecting microcalcifications, tiny calcium deposits that can be an early sign of ductal carcinoma in situ (DCIS), a precancerous condition. Digital mammography and digital breast tomosynthesis (3D mammography) have further improved detection rates, particularly in women with dense breasts.
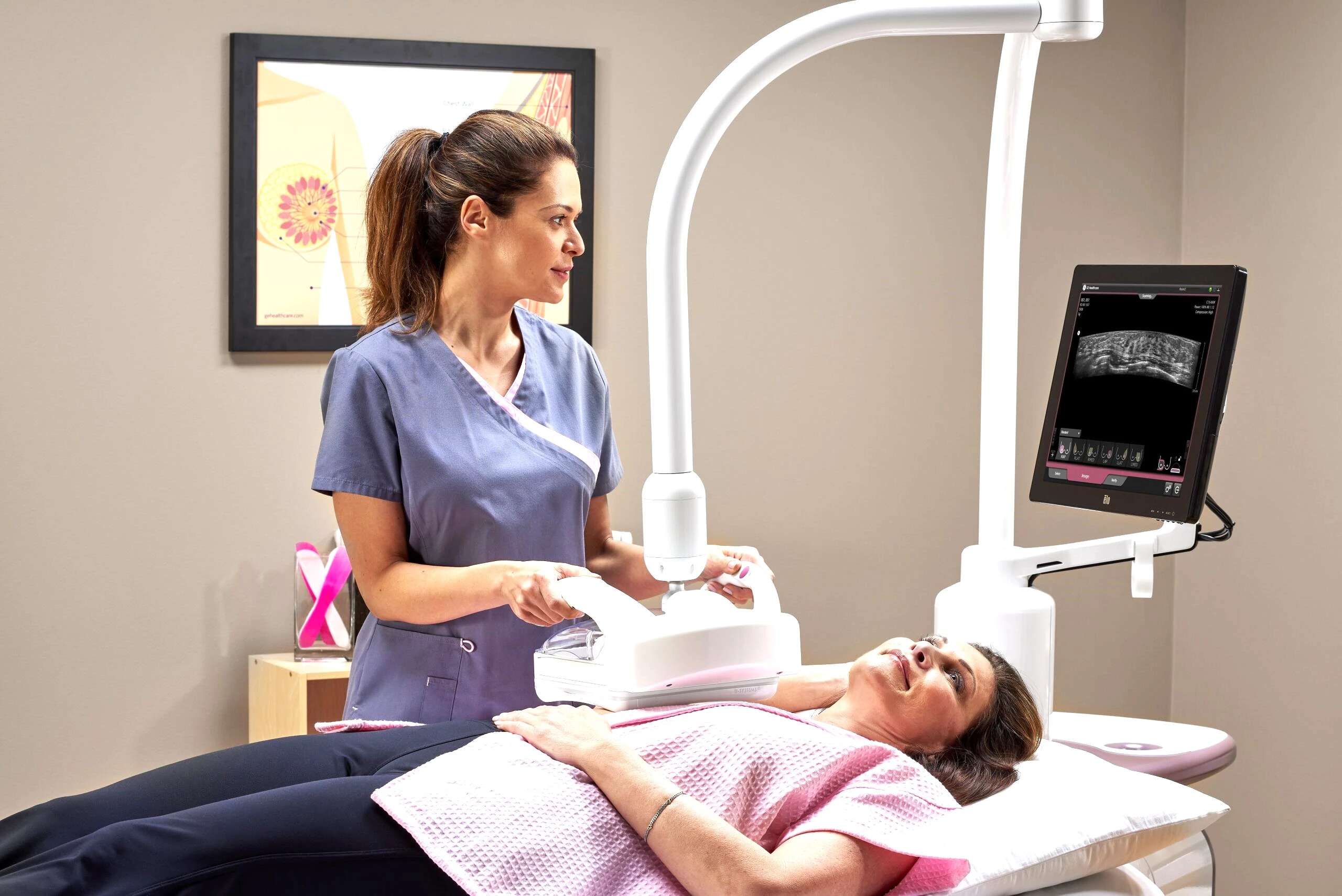
Breast ultrasound uses high-frequency sound waves to produce real-time images of the breast tissue without any radiation exposure. Our diagnostic ultrasound services include breast ultrasound, which is particularly valuable for evaluating palpable lumps, distinguishing solid masses from fluid-filled cysts, and examining women with dense breast tissue where mammographic sensitivity is reduced. Research published in the Journal of Clinical Oncology has shown that adding ultrasound to mammography can detect an additional 2 to 4 cancers per 1,000 women screened who have dense breasts.
| Feature | Mammogram | Breast Ultrasound |
|---|---|---|
| Technology | Low-dose X-ray imaging | High-frequency sound waves |
| Radiation | Low dose (approximately 0.4 mSv) | No radiation exposure |
| Primary strength | Detects microcalcifications and architectural distortions | Differentiates solid masses from cysts; evaluates dense breast tissue |
| Best for | Routine screening in women aged 40 and older | Supplementary screening for dense breasts; evaluating palpable lumps |
| Proven to reduce mortality | Yes (randomized controlled trials) | Not as a standalone screening tool |
| Sensitivity in dense breasts | Reduced (approximately 60-70%) | Higher (approximately 80-85%) |
| Can detect microcalcifications | Yes (key advantage) | No (significant limitation) |
| Duration | 10-15 minutes | 15-30 minutes |
| Discomfort | Brief breast compression required | No compression; minimal discomfort |
| When typically recommended | Annual screening from age 40 | When mammogram is inconclusive, for dense breasts, or for women under 40 |
Comparison of mammography and breast ultrasound for breast cancer screening. In many cases, both methods are used together for the most accurate evaluation.
For most women, mammography is the primary screening tool, with ultrasound serving as a valuable complement when additional information is needed. Women with extremely dense breast tissue, those with a strong family history of breast cancer, and women who are pregnant (where radiation must be avoided) may benefit from ultrasound as a first-line or primary imaging study. Your radiologist will recommend the most appropriate combination based on your individual risk profile, breast density, and clinical situation. Women should also discuss comprehensive breast health with their gynecology specialist, who can coordinate screening schedules and assess overall reproductive health alongside breast cancer risk.
Breast Cancer Screening Guidelines by Age
Breast cancer screening recommendations vary by age group and individual risk level. The following guidelines are based on recommendations from the American Cancer Society (ACS), the World Health Organization (WHO), and the UAE National Screening Program. Women with higher-than-average risk, such as those with BRCA mutations or a strong family history, may need to begin screening earlier and more frequently. You may also find our When to Start Mammograms: Age & Schedule Guide helpful.
Ages 20 to 39: Awareness and Clinical Examination
- Perform a monthly breast self-examination (BSE) starting at age 20 to become familiar with the normal look and feel of your breasts
- Have a clinical breast examination (CBE) by a healthcare professional every one to three years
- Discuss family history and personal risk factors with your doctor to determine if earlier screening imaging is warranted
- Women with BRCA1/BRCA2 mutations or a first-degree relative diagnosed before age 50 should consider annual breast MRI and/or mammography starting at age 25 to 30
Ages 40 to 49: Begin Annual Mammography
- Begin annual screening mammography at age 40
- Continue monthly breast self-examination
- Have an annual clinical breast examination
- If you have dense breast tissue (categories C or D on your mammogram report), discuss supplementary ultrasound screening with your doctor
Ages 50 to 74: Consistent Annual or Biennial Screening
- Continue annual or biennial (every two years) mammography, depending on individual risk assessment and physician recommendation
- Continue monthly breast self-examination and annual clinical breast examination
- Consider 3D mammography (digital breast tomosynthesis) for improved detection, especially if you have dense breasts
- Remain vigilant for any new breast changes between screening appointments
Ages 75 and Older: Individualized Screening
- Continue screening as long as overall health is good and life expectancy is at least 10 years
- Discuss the benefits and limitations of continued screening with your doctor based on your individual health status
Self-Examination: Monthly Breast Check Guide
A monthly breast self-examination (BSE) is a simple, no-cost practice that empowers women to detect changes in their breasts early. While BSE alone is not a substitute for mammographic screening, it plays an important role in overall breast health awareness. Studies published in The Lancet indicate that approximately 40% of breast cancers in women who receive screening are first detected by the women themselves as a palpable abnormality. The best time to perform BSE is seven to ten days after the start of your menstrual period, when breast tissue is least swollen and tender. Postmenopausal women should choose a consistent day each month.
Step-by-Step Self-Examination
- Step 1 - Visual inspection in the mirror: Stand undressed from the waist up in front of a mirror with your arms at your sides. Look at both breasts for any changes in size, shape, contour, skin texture, or nipple position. Repeat with your arms raised above your head, and then with your hands pressed firmly on your hips to flex your chest muscles. Look for dimpling, puckering, or asymmetry in all three positions
- Step 2 - Examine while standing or in the shower: Using the pads of your three middle fingers (not the fingertips), press firmly in small circular motions to feel the entire breast from the collarbone to the bra line and from the armpit to the breastbone. Use light pressure for tissue just beneath the skin, medium pressure for tissue in the middle, and firm pressure for tissue near the chest wall. Cover the entire breast in an up-and-down pattern (vertical strip method) for the most thorough examination
- Step 3 - Examine while lying down: Lie on your back with a pillow under the shoulder of the breast you are examining. This position spreads the breast tissue evenly over the chest wall, making it easier to feel deep abnormalities. Place the arm of the side being examined behind your head. Repeat the same circular motion pattern used in Step 2, covering the entire breast and armpit area
- Step 4 - Check the nipple: Gently squeeze each nipple between your thumb and index finger. Note any discharge (clear, bloody, or milky), pain, or change in nipple shape or direction
- Step 5 - Record and compare: If you notice any change from the previous month, including a new lump, thickening, skin change, discharge, or asymmetry, schedule an appointment with your doctor promptly. Do not wait until your next scheduled screening
"Self-examination is not about finding cancer; it is about knowing your own body well enough to recognize when something has changed," says Dr. Osama Elzamzami, Head of Radiology at DCDC. "A woman who regularly examines her breasts can detect a new lump or change weeks or months before her next screening appointment, and that early detection can save her life."
Breast Cancer Screening in Dubai
Dubai has made significant investments in cancer screening infrastructure, with breast cancer screening services available at government hospitals, private clinics, and specialized diagnostic centers throughout the emirate. The Dubai Health Authority (DHA) actively promotes breast cancer awareness through annual campaigns, free screening initiatives during Breast Cancer Awareness Month (October), and the Basmah Cancer Screening Program, which provides subsidized screening for eligible residents.
Breast Screening at DCDC Dubai Healthcare City
DCDC (Doctors Clinic Diagnostic Center) in Dubai Healthcare City offers comprehensive breast cancer screening services in a comfortable, patient-centered environment. The center is equipped with advanced digital mammography and high-resolution breast ultrasound technology, and all imaging is interpreted by experienced consultant radiologists who specialize in breast imaging and diagnostic radiology.
- Digital mammography: Full-field digital mammography with optimized compression protocols designed for patient comfort while maintaining diagnostic image quality
- Breast ultrasound: High-resolution ultrasound for evaluating palpable lumps, assessing dense breast tissue, and guiding further investigation when mammographic findings require clarification
- Same-day results: In most cases, the radiologist's report is available on the same day as the examination, reducing the anxiety associated with waiting for results
- Experienced radiology specialists: All breast imaging at DCDC is performed and interpreted by consultant radiologists with extensive experience in breast diagnostic imaging
- Convenient location: DCDC is located in Dubai Healthcare City, easily accessible from Oud Metha, Karama, Bur Dubai, Downtown Dubai, and the wider UAE, with ample parking and public transport access
Patient Awareness Story
A 47-year-old expatriate living in Dubai had been postponing her mammogram for over three years due to a busy work schedule and the assumption that she was "too young and healthy" to be at risk. When her company offered a health screening program, she decided to have a mammogram at DCDC. The mammogram revealed a cluster of suspicious microcalcifications in her left breast that were completely undetectable by touch. A subsequent biopsy confirmed ductal carcinoma in situ (DCIS), a stage 0 pre-invasive breast cancer that had not yet spread beyond the milk ducts.
"This patient's case is a perfect example of why screening matters," says Dr. Osama Elzamzami, Head of Radiology at DCDC. "The microcalcifications were invisible on physical examination and would not have been detected by ultrasound alone. The mammogram caught this at the earliest possible stage, before it had any opportunity to become invasive. She underwent a minimally invasive procedure and is now cancer-free with an excellent long-term prognosis."
This experience motivated her to become an advocate for breast screening among her colleagues and friends, sharing her story to encourage other women not to delay their mammograms. Her message is simple: a 15-minute screening appointment can save your life.
How to Book a Breast Screening at DCDC
Booking a breast cancer screening at DCDC is straightforward. Appointments can be made by phone, WhatsApp, or through the online booking form. No referral is required for a screening mammogram or breast ultrasound. Walk-in patients are accommodated subject to availability, though booking in advance is recommended to minimize waiting time. DCDC accepts most major insurance plans in the UAE, and self-pay options are available for uninsured patients.
Schedule Your Breast Screening Today
Do not wait for symptoms to appear. At DCDC in Dubai Healthcare City, our experienced radiology team provides comprehensive breast cancer screening with digital mammography and breast ultrasound. Same-day results, compassionate care, and a commitment to early detection.
Or WhatsApp us directly for a quick appointment.
Related Services at DCDC
Expert care and advanced diagnostics at Dubai Healthcare City
Frequently Asked Questions
Final Thoughts
Breast cancer remains the most common cancer in women, but it is also one of the most survivable when detected early. The 10 warning signs outlined in this guide are not meant to cause alarm but to empower every woman with the knowledge needed to recognize changes that warrant medical attention. The combination of breast self-awareness, regular clinical examinations, and age-appropriate screening mammography forms a powerful defense against late-stage diagnosis. When breast cancer is found at stage I, the survival rate exceeds 99%, a statistic that speaks directly to the life-saving value of early detection.
If you are due for a screening, have noticed any changes in your breasts, or simply want peace of mind, scheduling a mammogram is one of the most important health decisions you can make. At Doctors Clinic Diagnostic Center in Dubai Healthcare City, our experienced radiology team is committed to providing accurate, compassionate, and timely breast cancer screening services. Do not let a busy schedule, fear of the procedure, or the assumption that "it cannot happen to me" delay your screening. Early detection saves lives, and a 15-minute appointment could make all the difference.
Sources & References
This article was reviewed by our medical team and references the following sources:
- World Health Organization - Breast Cancer Facts
- American Cancer Society - Breast Cancer Screening Guidelines
- National Cancer Institute - Breast Cancer Screening (PDQ)
- The Lancet - Breast Cancer Screening: An Updated Review of Evidence on Benefits and Harms
- Dubai Health Authority - Basmah Cancer Screening Program
Medical content on this site is reviewed by DHA-licensed physicians. See our editorial policy for more information.
Related Articles
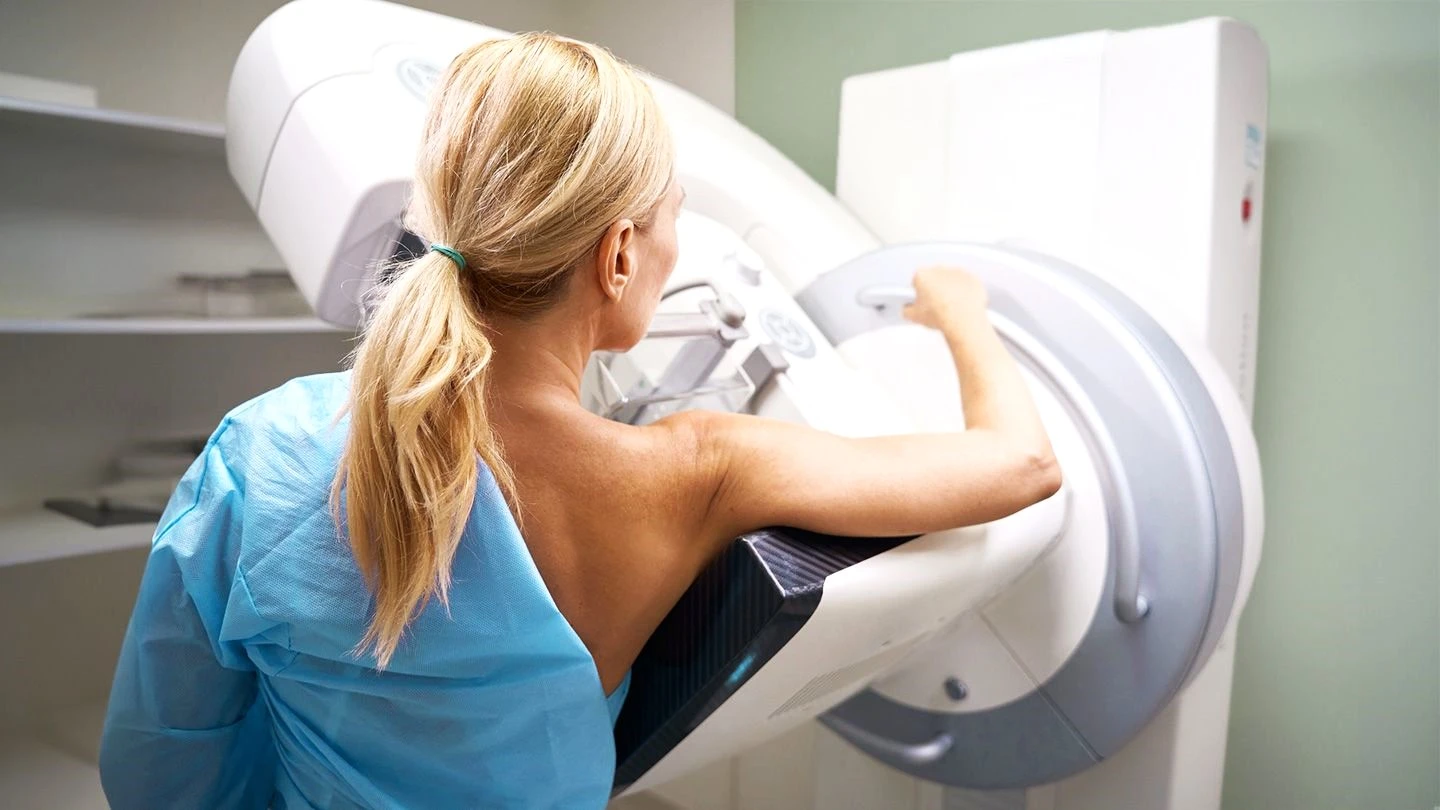
Mammogram in Dubai: Complete Guide to Screening, Procedure, Results & Breast Density

Mammogram Cost in Dubai: Prices, Insurance & Free Options
Women's Health Screening Guide
More in Women's Health

Perimenopause Symptoms Dubai: Signs & Care (2026)
Read More
Pregnancy Scan Schedule Dubai: Trimester Guide (2026)
Read More
PCOS Treatment Dubai: Diagnosis & Care (2026)
Read More
HPV Test Dubai: Types, Cost & Screening (2026)
Read More
NT Scan Dubai: Cost, Timing & Results (2026)
Read More
Pregnancy After HSG Test Dubai: Success Rates (2026)
Read More© 2026 Doctors Clinic Diagnostic Center (DCDC), Dubai Healthcare City. Originally published at https://doctorsclinicdubai.ae/blog/breast-cancer-early-signs-symptoms. All rights reserved. Unauthorized reproduction is prohibited.