نکات کلیدی
- All women should begin annual mammogram screening at age 40, regardless of risk factors — this is when breast cancer incidence begins rising significantly
- Women with high-risk factors (BRCA mutation, first-degree family history, prior chest radiation) should start screening as early as age 30, typically with mammogram plus breast MRI
- Breast cancer is the most common cancer among women in the UAE, and UAE women are diagnosed at a younger average age (48) than women in Western countries (62)
- Mammograms detect breast cancer up to 3 years before a lump becomes palpable, when the 5-year survival rate exceeds 99% for localized disease
- For women with dense breast tissue, supplemental breast ultrasound alongside mammography improves cancer detection rates by approximately 40%
One of the most common questions women ask their doctor is: “When should I start getting mammograms?” The answer depends on your age, family history, and personal risk factors. For most women, annual mammogram screening should begin at age 40. For women with elevated risk, screening may need to start at 30 or even earlier. This guide explains exactly when to start, how often to screen, what risk factors accelerate the timeline, and how mammograms compare to other breast screening methods.
Breast cancer is the most common cancer among women in the UAE, and UAE women are diagnosed at an average age of 48 — significantly younger than the global average of 62. This makes age-appropriate screening particularly critical for women living in Dubai and the wider region. Understanding the screening schedule, knowing your risk category, and choosing the right imaging approach can genuinely save your life.
When to Start Mammogram Screening
Major medical organizations have slightly different recommendations, but the consensus is clear: regular mammogram screening saves lives. The American College of Radiology (ACR), the American Cancer Society (ACS), and the Dubai Health Authority all recommend that women begin annual mammography between ages 40 and 45, with earlier screening for high-risk women.
| Risk Category | Start Screening | Frequency | Additional Imaging |
|---|---|---|---|
| Average risk (no family history, no known mutations) | Age 40 | Annually | None required |
| Moderate risk (first-degree relative diagnosed after age 50) | Age 35–40 | Annually | Consider breast ultrasound for dense breasts |
| High risk (BRCA1/2 mutation carrier) | Age 25–30 | Annually | Alternating mammogram and breast MRI every 6 months |
| High risk (chest radiation before age 30, e.g. for lymphoma) | Age 25 or 8 years post-radiation | Annually | Breast MRI recommended in addition to mammogram |
| High risk (first-degree relative diagnosed before age 50) | Age 30 or 10 years before relative’s diagnosis age | Annually | Consider breast MRI if lifetime risk >20% |
| Age 55+ | Continue screening | Annually or every 2 years based on discussion with doctor | Based on individual risk and breast density |
Based on ACR, ACS, and NCCN guidelines. Individual recommendations may vary based on personal risk assessment.
If you are unsure of your risk category, schedule a consultation with your doctor at DCDC. A simple risk assessment based on your family history, personal health history, and breast density can determine the right screening start age and frequency for you.
Mammogram Screening Frequency by Age
Ages 30–39 (High-Risk Women Only)
Routine mammogram screening is not recommended for average-risk women under 40 because breast cancer incidence is relatively low in this age group and younger breast tissue is denser, which can reduce mammogram sensitivity. However, women identified as high risk — BRCA1/2 carriers, those with prior chest radiation therapy, or those with a strong first-degree family history — should begin annual screening at age 25–30. High-risk screening typically combines annual mammography with annual breast MRI, often alternated every 6 months to provide semi-annual imaging coverage.
Ages 40–49: Annual Screening Begins
This is the decade when all women should begin annual mammogram screening, regardless of risk factors. Breast cancer incidence rises sharply after age 40, and annual mammography has been shown to reduce breast cancer mortality by approximately 40% in women aged 40–49 who screen regularly. Do not wait for your doctor to suggest it — if you are 40 and have not had a mammogram, book one now.
For women with dense breasts (identified on your first mammogram report), your radiologist may recommend supplemental breast ultrasound in addition to mammography. Dense tissue can mask small cancers on mammograms, and ultrasound can detect cancers that mammography alone misses.
Ages 50–74: Continued Annual or Biennial Screening
Breast cancer incidence continues to rise through the 50s, 60s, and 70s. Most guidelines recommend continuing annual mammography through at least age 74. Some organizations suggest switching to biennial (every 2 years) screening after age 55 for average-risk women, but this should be a shared decision with your doctor based on your individual risk profile, health status, and preferences. Women with ongoing risk factors (family history, dense breasts, prior breast biopsies) should continue annual screening.
Ages 75+: Individualized Decision
There is no upper age limit for mammogram screening, but the decision to continue should be based on overall health, life expectancy, and personal preferences. Women in good health with a life expectancy of 10+ years are generally advised to continue screening. Your doctor can help you weigh the benefits against the risks of potential over-diagnosis.
Risk Factors That Accelerate Mammogram Screening
Certain factors significantly increase your lifetime risk of breast cancer and may warrant earlier and more intensive screening. Understanding your risk category is essential for determining the right screening strategy.
- BRCA1 / BRCA2 gene mutations: Women carrying these mutations have a 45–72% lifetime risk of developing breast cancer (compared to 12.5% average risk). BRCA carriers should begin screening at age 25–30 with both mammogram and breast MRI
- First-degree family history: Having a mother, sister, or daughter diagnosed with breast cancer approximately doubles your risk. If the relative was diagnosed before age 50, screening should begin 10 years before her age at diagnosis
- Prior chest radiation: Women who received radiation therapy to the chest between ages 10 and 30 (typically for Hodgkin lymphoma) have a significantly elevated breast cancer risk and should begin screening by age 25 or 8 years after radiation, whichever comes later
- Dense breast tissue: Women with extremely dense breasts (category D on mammography) have a 4–6 times higher risk of breast cancer compared to women with fatty breasts. Dense tissue also makes cancers harder to detect on mammography, necessitating supplemental screening with ultrasound or MRI
- Personal history of breast conditions: Atypical ductal hyperplasia (ADH), atypical lobular hyperplasia (ALH), or lobular carcinoma in situ (LCIS) found on previous biopsies increase future breast cancer risk and may warrant more frequent screening
- Hormonal factors: Early menstruation (before age 12), late menopause (after age 55), first pregnancy after age 30, and never having been pregnant are all associated with modestly increased breast cancer risk due to prolonged estrogen exposure
Book Your Mammogram
Schedule your mammogram screening at DCDC Dubai Healthcare City. Walk-in and same-day appointments available.
BRCA Genetic Testing: Should You Get Tested?
BRCA1 and BRCA2 are genes that produce proteins involved in DNA repair. When these genes are mutated, they cannot function properly, significantly increasing the risk of breast cancer (45–72% lifetime risk) and ovarian cancer (10–44% lifetime risk). BRCA testing is a simple blood test that identifies whether you carry these mutations.
BRCA testing is not recommended for everyone. It is most appropriate for women with specific risk indicators.
- Two or more close relatives diagnosed with breast cancer, especially before age 50
- A family member with both breast and ovarian cancer
- A male relative with breast cancer
- A known BRCA mutation in the family
- Ashkenazi Jewish heritage (BRCA mutations are more prevalent in this population)
- Triple-negative breast cancer diagnosed before age 60
If BRCA testing reveals a mutation, it does not mean you will definitely develop breast cancer. It means your risk is significantly higher than average, and you should work with your doctor to create an enhanced screening and risk-reduction plan. Options include starting mammogram and MRI screening at age 25–30, risk-reducing medications (tamoxifen, raloxifene), or, in some cases, preventive surgery. DCDC offers genetic testing services including BRCA analysis.
Mammogram vs Breast Ultrasound: Which Do You Need?
Mammography and breast ultrasound are complementary imaging tools, not alternatives. Each has distinct strengths, and many women benefit from both.
| Factor | Mammogram | Breast Ultrasound |
|---|---|---|
| Primary purpose | Screening tool for all women age 40+ | Supplemental screening for dense breasts; characterizing lumps |
| Best at detecting | Calcifications, architectural distortions, masses in fatty tissue | Masses in dense tissue, distinguishing solid from cystic lumps |
| Radiation | Very low-dose X-ray | No radiation (uses sound waves) |
| Dense breasts | Sensitivity reduced (cancers can be hidden) | Excellent for dense tissue; detects cancers mammography misses |
| Standalone screening | Yes — gold standard for breast cancer screening | No — not recommended as sole screening tool |
| Duration | 15–20 minutes | 15–30 minutes |
| Compression | Required (brief discomfort) | No compression needed |
Mammography remains the gold standard for breast cancer screening. Ultrasound is used as a complement, not a replacement.
The key message is: mammography is the proven screening tool that saves lives. Breast ultrasound is valuable as a supplement for women with dense breasts and for evaluating specific lumps or areas of concern identified on mammography or clinical exam. Breast MRI is reserved for high-risk women and offers the highest sensitivity of any imaging modality but has a higher false-positive rate and is more expensive.
At DCDC, our radiologists assess your breast density on your mammogram and recommend supplemental imaging if appropriate. If you have been told you have dense breasts, ask about adding a breast ultrasound to your annual screening.
What to Expect During a Mammogram
Many women delay their first mammogram because of anxiety about the procedure. Understanding what actually happens helps reduce that anxiety. A mammogram is a quick, safe procedure that takes about 15–20 minutes from start to finish.
- Before: Avoid applying deodorant, antiperspirant, powder, or lotion to your chest or underarm area on the day of the exam — these products can appear as white spots on the images. Wear a two-piece outfit so you only need to remove your top. Schedule your mammogram for 1–2 weeks after your period when breasts are least tender
- During: You stand in front of the mammography machine. The technologist positions one breast at a time on a flat plate, and a second plate presses down briefly to compress the breast. Compression is necessary to spread the tissue evenly, reduce motion blur, and lower the radiation dose. Two images of each breast are standard: top-to-bottom and side-to-side. The compression lasts only 3–5 seconds per image and may be uncomfortable but should not be painful
- After: You can dress and leave immediately. Results at DCDC are reported within 24–48 hours by a consultant radiologist. If any area needs further evaluation, you will be contacted for additional imaging (magnification views, spot compression, or ultrasound). Being recalled does not mean you have cancer — most callbacks result in normal findings after additional views
If you experienced pain during a previous mammogram, tell the technologist. Adjusting compression pressure, timing your exam with your menstrual cycle, and using a slower compression technique can all improve comfort significantly.
Schedule Your Breast Screening
Book your mammogram at DCDC Dubai Healthcare City. Digital mammography with results within 24–48 hours.
خدمات مرتبط در DCDC
مراقبت تخصصی و تشخیص پیشرفته در شهر بهداشت دبی
سؤالات متداول
Early Screening Saves Lives
Breast cancer caught at stage I — before it has spread beyond the breast — has a 99% five-year survival rate. Caught at stage IV, that rate drops below 30%. The difference between these outcomes is often a single mammogram that detected a cancer too small to feel. Annual mammogram screening starting at age 40 is the single most effective strategy for catching breast cancer early.
For women in the UAE, screening is especially important. Breast cancer is the most commonly diagnosed cancer among women in the region, and UAE women tend to be diagnosed at a younger age than women in Western countries. If you have not had a mammogram and you are over 40 — or if you have risk factors that warrant earlier screening — the time to act is now.
At DCDC Dubai Healthcare City, we offer digital mammography with results reported by an experienced consultant radiologist within 24–48 hours. Breast ultrasound is available as a complementary screening tool for women with dense breasts. Contact our team to book your mammogram and take the single most important step in breast cancer prevention.
منابع و مراجع
این مقاله توسط تیم پزشکی ما بررسی شده و به منابع زیر ارجاع میدهد:
- American Cancer Society — Breast Cancer Screening Guidelines
- American College of Radiology — ACR Breast Cancer Screening Recommendations
- National Comprehensive Cancer Network — NCCN Breast Cancer Screening Guidelines
- Dubai Health Authority — Cancer Screening Program
- World Health Organization — Breast Cancer: Prevention and Control
محتوای پزشکی این سایت توسط پزشکان دارای مجوز DHA بررسی میشود. مشاهده سیاست تحریریه برای اطلاعات بیشتر.
Related Articles

Mammogram Cost in Dubai: Complete Pricing Guide
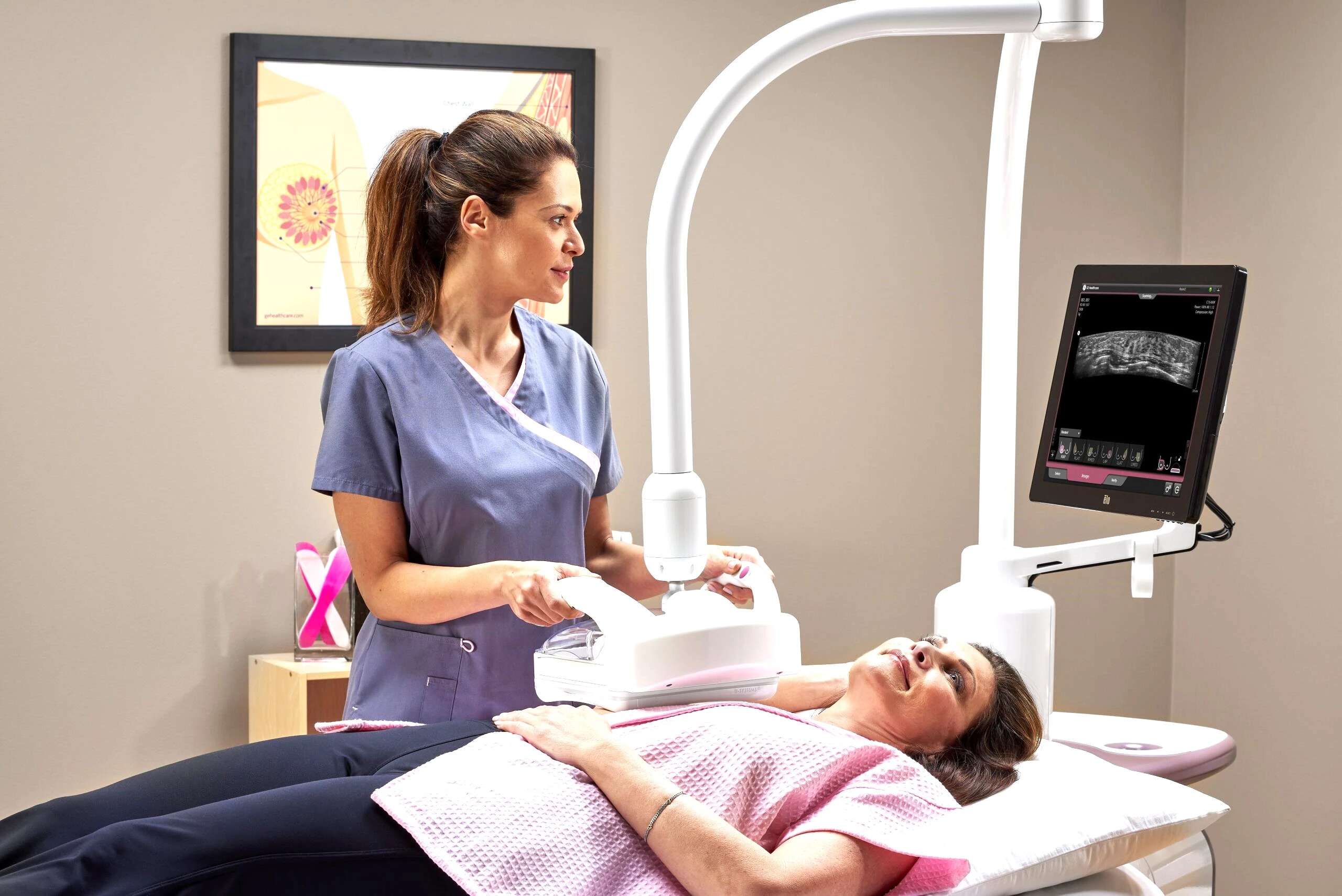
Breast Cancer Early Signs & Symptoms
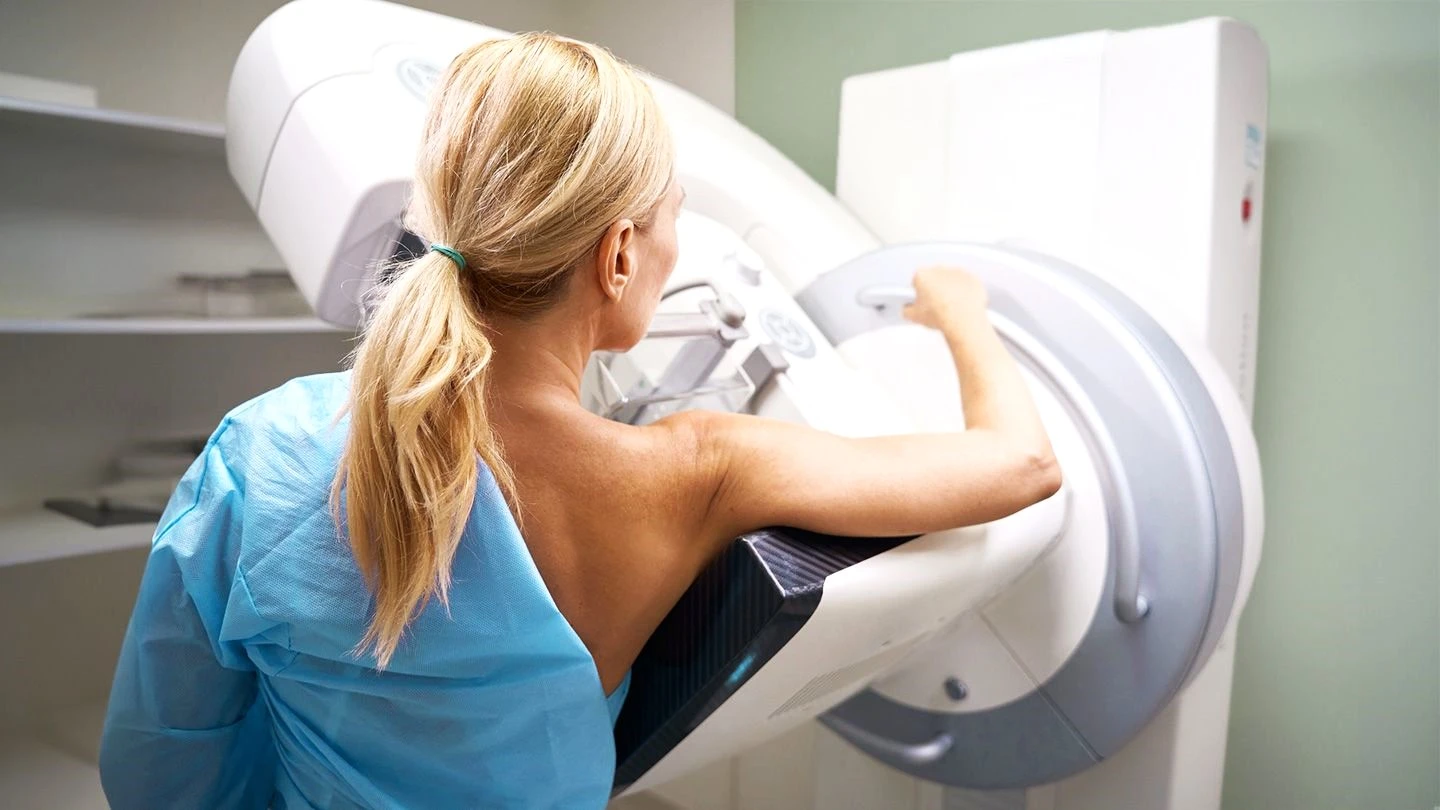
Breast Cancer Screening Guide
Cancer Screening in Dubai: Complete Guide
blogPage.moreFromCategory

Pregnancy After HSG Test Dubai: Success Rates (2026)
بیشتر بخوانید
NIPT vs Amniocentesis: Which Test to Choose (2026)
بیشتر بخوانید
NIPT Results: High-Risk vs Low-Risk Explained (2026)
بیشتر بخوانید
NIPT Test Dubai: Cost, Accuracy & Timing (2026)
بیشتر بخوانید
Cervical Cancer Screening Dubai: Pap Smear & HPV (2026)
بیشتر بخوانید
Best Menopause Doctor Dubai: How to Choose (2026)
بیشتر بخوانید© 2026 Doctors Clinic Diagnostic Center (DCDC), Dubai Healthcare City. Originally published at https://doctorsclinicdubai.ae/blog/mammogram-screening-age-guide. All rights reserved. Unauthorized reproduction is prohibited.


