Mga Pangunahing Punto
- Individual testosterone tests at DCDC Dubai Healthcare City start from AED 200, with full male hormone panels from AED 750 and results in 24–48 hours.
- Normal total testosterone for adult men ranges from 300 to 1,000 ng/dL (10.4–34.7 nmol/L) — two low morning readings are required before diagnosing hypogonadism.
- Testosterone blood draws must be performed between 7 and 10 AM because levels follow a circadian rhythm and can drop 20–30% by the afternoon.
- Approximately 40% of men over 45 have clinically low testosterone, and prevalence is increasing in younger men due to obesity, stress, and metabolic conditions.
- Testosterone testing is not only for men — women need it for diagnosing PCOS, evaluating hirsutism, and investigating fertility issues.
- DCDC offers integrated care in Dubai Healthcare City: your testosterone results are reviewed by a GP and, when needed, referred to a urologist or endocrinologist in the same building.
Testosterone influences far more than libido — it regulates muscle mass, bone density, red blood cell production, fat distribution, mood, and cognitive function in both men and women. When levels fall outside the normal range, the consequences can affect nearly every system in the body. Hormone testing at DCDC in Dubai Healthcare City offers individual testosterone tests from AED 200 and comprehensive male hormone panels from AED 750, with morning appointments available seven days a week and results typically within 24–48 hours.
This guide covers everything you need to know about testosterone testing in Dubai: the different test types, normal ranges by age and sex, symptoms that warrant testing, how to prepare, what results mean, what it costs, and when to see a specialist.
What Is a Testosterone Test and Why Does It Matter?
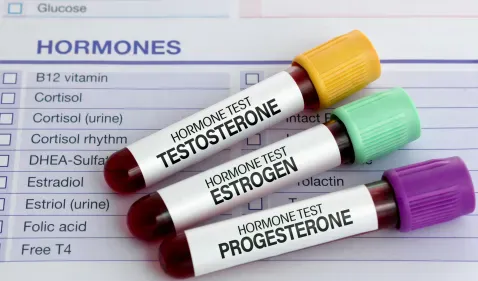
A testosterone test is a blood test that measures the concentration of testosterone — the primary androgen hormone — circulating in your bloodstream. In men, testosterone is produced mainly by the Leydig cells of the testes under the control of luteinising hormone (LH) from the pituitary gland. In women, smaller amounts are produced by the ovaries and adrenal glands. The test is ordered to evaluate suspected hormonal deficiencies, monitor replacement therapy, investigate infertility, and assess conditions such as polycystic ovary syndrome (PCOS).
Testosterone matters because it is the master regulator of male development and health. It drives muscle protein synthesis, maintains bone mineral density, stimulates red blood cell production in the bone marrow, regulates fat metabolism, supports sperm production, and influences mood and cognitive function. In women, testosterone contributes to libido, energy levels, and musculoskeletal health, though in much lower concentrations. When testosterone levels fall too low — or climb too high — the downstream effects can be significant and wide-ranging.
The clinical importance of testosterone testing has grown considerably in recent years. Research shows that approximately 40% of men over the age of 45 have testosterone levels below the normal threshold, and the prevalence of low testosterone in younger men is increasing alongside rising rates of obesity, type 2 diabetes, and chronic stress. In the UAE specifically, high rates of vitamin D deficiency, sedentary lifestyles, and metabolic syndrome make testosterone assessment a particularly relevant part of men's health screening.
When Should You Get Your Testosterone Levels Checked in Dubai?
Not every man needs a routine testosterone test, but certain symptoms and risk factors should prompt evaluation. The Endocrine Society recommends testosterone testing for men presenting with specific clinical signs rather than as a universal screening tool. However, given the high prevalence of modifiable risk factors in Dubai's population, proactive testing is increasingly common and clinically justified.
Signs That Warrant Testing in Men
- Persistent fatigue or low energy that does not improve with adequate sleep
- Reduced sex drive or difficulty maintaining erections
- Loss of muscle mass or strength despite regular exercise
- Increased body fat, particularly around the abdomen
- Mood changes including irritability, low motivation, or depression
- Difficulty concentrating or memory problems (often described as brain fog)
- Decreased bone density or unexplained fractures
- Reduced body or facial hair growth
- Hot flashes or night sweats
- Infertility or low sperm count
Risk Factors That Increase the Likelihood of Low Testosterone
- Obesity: Excess adipose tissue converts testosterone to oestrogen via the aromatase enzyme, creating a vicious cycle of declining testosterone and increasing fat accumulation
- Type 2 diabetes: Men with diabetes have approximately double the risk of low testosterone compared to non-diabetic men
- Obstructive sleep apnoea: Disrupted sleep architecture suppresses the nocturnal testosterone production that accounts for the morning peak
- Chronic opioid use: Opioid medications suppress the hypothalamic-pituitary-gonadal axis, often resulting in clinically significant testosterone deficiency
- Chronic stress: Elevated cortisol directly suppresses gonadotropin-releasing hormone (GnRH), reducing LH and consequently testosterone production
- Age over 40: Testosterone declines by roughly 1–2% per year after age 30, though this alone rarely causes symptomatic deficiency
Types of Testosterone Tests Explained
When your doctor orders a testosterone test, the request may include one or more of several distinct measurements. Each provides different clinical information, and a comprehensive assessment typically requires more than just a total testosterone level.
Total Testosterone
Total testosterone measures all testosterone in the blood — both bound and unbound. Approximately 98% of circulating testosterone is bound to proteins: about 60–70% to sex hormone-binding globulin (SHBG) and 30–40% to albumin. Only 1–2% circulates freely. Total testosterone is the first-line screening test and the number most commonly referenced in clinical guidelines. Normal values for adult men range from 300 to 1,000 ng/dL (10.4–34.7 nmol/L).
Free Testosterone
Free testosterone measures only the unbound fraction — the 1–2% of testosterone that is immediately available to enter cells and exert biological effects. Normal free testosterone for men aged 20–50 ranges from 5 to 21 pg/mL. Free testosterone is particularly important when SHBG levels are abnormal (elevated in liver disease, hyperthyroidism, or ageing; decreased in obesity, diabetes, or hypothyroidism) because total testosterone can appear normal while the biologically active fraction is low.
Bioavailable Testosterone
Bioavailable testosterone includes both free testosterone and the portion loosely bound to albumin (since albumin-bound testosterone can dissociate and become active). It represents approximately 30–40% of total testosterone and provides a more complete picture of functional testosterone status than free testosterone alone, particularly in older men.
SHBG (Sex Hormone-Binding Globulin)
SHBG is a protein produced by the liver that binds testosterone tightly, rendering it biologically inactive. SHBG levels are critical for interpreting testosterone results accurately. High SHBG means more testosterone is bound and unavailable — a man can have a normal total testosterone but low free testosterone if SHBG is elevated. Conditions that raise SHBG include ageing, liver disease, and hyperthyroidism. Conditions that lower SHBG include obesity, type 2 diabetes, and hypothyroidism.
Understanding the different types of testosterone tests is essential for accurate diagnosis. If you are exploring broader hormone testing in Dubai, a full male hormone panel that includes total testosterone, free testosterone, SHBG, LH, and FSH provides the most complete clinical picture.
Normal Testosterone Levels by Age: What the Numbers Mean
Testosterone levels vary significantly by age, time of day, and individual physiology. The following reference ranges are based on the Endocrine Society guidelines and represent morning values drawn between 7 and 10 AM, which is when testosterone peaks due to circadian rhythmicity.
| Age Group | Total Testosterone (ng/dL) | Free Testosterone (pg/mL) | Clinical Notes |
|---|---|---|---|
| 18–25 years | 400–1,000 | 9–21 | Peak testosterone production; highest baseline levels |
| 26–35 years | 350–900 | 8–19 | Levels remain relatively stable through early 30s |
| 36–45 years | 300–800 | 6–17 | Gradual decline begins; 1–2% decrease per year typical |
| 46–55 years | 250–700 | 5–15 | ~40% of men in this bracket have levels below 300 ng/dL |
| 56–65 years | 200–600 | 4–13 | Symptoms more common even within 'normal' range |
| Over 65 years | 150–500 | 3–10 | Lower thresholds may be accepted; symptom correlation key |
Typical testosterone reference ranges by age for men (morning values)
It is important to understand that these ranges are population averages, not strict boundaries. The Endocrine Society uses 300 ng/dL as the diagnostic threshold for hypogonadism, but clinical context matters. A 30-year-old man with a total testosterone of 310 ng/dL and significant symptoms may warrant treatment, whereas a 65-year-old man at 280 ng/dL with no symptoms may not. Two separate morning blood draws showing low levels are required before a formal diagnosis of hypogonadism is made.
Symptoms of Low Testosterone in Men
Low testosterone (hypogonadism) produces a constellation of symptoms that can develop gradually over months or years, making them easy to dismiss as normal ageing or lifestyle-related fatigue. Recognising these symptoms is the first step toward getting tested and treated.
Sexual Symptoms
- Reduced libido: One of the earliest and most consistent symptoms. Men often describe a noticeable drop in sexual interest that is disproportionate to their age.
- Erectile dysfunction: While ED has many causes (vascular, neurological, psychological), testosterone deficiency is a contributing factor in 20–30% of cases.
- Reduced morning erections: The absence of spontaneous morning erections can be an early indicator of declining testosterone.
- Decreased ejaculate volume: Testosterone stimulates the seminal vesicles; low levels can reduce semen production.
Physical Symptoms
- Loss of muscle mass and strength: Testosterone is anabolic — it promotes muscle protein synthesis. Men with low T often notice progressive weakness and muscle wasting.
- Increased body fat: Particularly around the abdomen. Low testosterone promotes fat accumulation and fat tissue produces aromatase, which converts testosterone to oestrogen, worsening the deficiency.
- Decreased bone density: Testosterone maintains bone mineral density. Severe or prolonged deficiency increases fracture risk.
- Gynaecomastia: Breast tissue development due to a shift in the testosterone-to-oestrogen ratio.
- Fatigue: A deep, persistent tiredness that does not resolve with rest.
Cognitive and Emotional Symptoms
- Depressed mood: Low testosterone is associated with increased rates of depressive symptoms, irritability, and emotional flatness.
- Difficulty concentrating: Often described as brain fog — trouble focusing, poor memory, and reduced mental sharpness.
- Reduced motivation: A general loss of drive and ambition that goes beyond normal fluctuations in energy.
- Sleep disturbances: Insomnia or poor sleep quality, which can further suppress testosterone production in a self-reinforcing cycle.
If you recognise several of these symptoms, a testosterone blood test can provide clarity. Many of these symptoms overlap with other conditions — thyroid disorders, depression, sleep apnoea, and iron deficiency can all present similarly. That is why comprehensive blood tests in Dubai that include a metabolic panel alongside hormone testing are often recommended to rule out concurrent issues.
Testosterone Testing for Women: PCOS, Fertility and Beyond
While testosterone is often thought of as a male hormone, it plays important roles in women's health as well. Women produce testosterone in the ovaries and adrenal glands at roughly one-tenth the concentration found in men. Abnormal testosterone levels in women — whether too high or too low — can cause significant clinical problems.
High Testosterone in Women
Elevated testosterone in women is most commonly associated with polycystic ovary syndrome (PCOS), which affects 10–15% of women of reproductive age. Symptoms include irregular periods, acne, hirsutism (excess facial and body hair), scalp hair thinning, and difficulty conceiving. The hormone panel for suspected PCOS typically includes total and free testosterone, DHEA-S, androstenedione, fasting insulin, and sometimes 17-hydroxyprogesterone to exclude congenital adrenal hyperplasia.
Low Testosterone in Women
Low testosterone in women can contribute to reduced libido, chronic fatigue, loss of muscle tone, and decreased bone density. This is particularly relevant during and after menopause, when both oestrogen and testosterone decline. Some clinicians include testosterone in menopausal hormone panels, although female testosterone deficiency remains an area of evolving research.
Fertility Implications
In women undergoing fertility evaluation, testosterone levels help assess ovarian function and guide treatment decisions. Elevated testosterone can interfere with ovulation and is one of the diagnostic criteria for PCOS under the Rotterdam criteria. Treatment to lower testosterone (through lifestyle modification, metformin, or anti-androgen medications) can restore ovulatory cycles in many women with PCOS-related infertility.
How to Prepare for Your Testosterone Blood Test
Preparation for a testosterone test is straightforward, but following the correct protocol is essential for accurate results. Incorrect timing or preparation is one of the most common causes of misleading testosterone values.
Essential Preparation Steps
- Schedule a morning appointment (7–10 AM): Testosterone peaks in the early morning due to circadian rhythm. Afternoon testing can yield values 20–30% lower than your true baseline.
- Fasting is not typically required: Unlike glucose or lipid tests, testosterone testing does not require an overnight fast. However, if your doctor has ordered a full panel that includes fasting glucose or insulin, you should fast for 8–12 hours.
- Get adequate sleep the night before: Sleep deprivation acutely suppresses testosterone. One study found that one week of restricted sleep (5 hours per night) reduced testosterone by 10–15%.
- Avoid intense exercise 24 hours before: Strenuous exercise can temporarily elevate testosterone, potentially giving a falsely reassuring result.
- Inform your doctor of all medications: Opioids, corticosteroids, anti-androgens, and some antidepressants can all affect testosterone levels.
- Avoid alcohol for 24 hours before: Alcohol acutely suppresses testosterone production and can skew results.
- Manage stress where possible: Acute stress elevates cortisol, which suppresses testosterone. Arrive at the clinic with enough time to sit calmly for a few minutes before your blood draw.
At DCDC, our phlebotomy team draws testosterone samples as a simple venous blood draw from the arm — the same process as any standard blood test. Results are typically available within 24–48 hours. For women, testosterone can be tested on any day of the menstrual cycle, though your doctor may coordinate it with other hormone tests that are cycle-dependent.
Many patients also choose to combine their testosterone test with other health assessments. Hair loss treatment options in Dubai often begin with hormone evaluation, as both low testosterone in men and high testosterone in women are associated with different patterns of hair thinning.
Testosterone Test Cost in Dubai: Pricing Comparison (2026)
The cost of testosterone testing in Dubai depends on whether you are ordering an individual test or a comprehensive male hormone panel, and whether you are using insurance or paying out of pocket. Prices vary across facilities, from hospital laboratories to independent diagnostic centres.
| Test / Panel | DCDC Price | Dubai Market Range |
|---|---|---|
| Total testosterone (individual) | From AED 200 | AED 150–500 |
| Free testosterone (individual) | From AED 200 | AED 150–500 |
| SHBG (sex hormone-binding globulin) | From AED 200 | AED 150–400 |
| Full male hormone panel (total & free T, SHBG, FSH, LH, estradiol) | From AED 750 | AED 500–2,000 |
| GP consultation (results review) | From AED 150 | AED 150–500 |
| Comprehensive men's health panel (hormones + metabolic + vitamins) | From AED 1,500 | AED 1,000–3,000 |
Testosterone test pricing comparison in Dubai (2026)
DCDC accepts direct billing with over 20 major insurance providers in Dubai including Daman, AXA, Bupa, Cigna, and MetLife. When hormone testing is ordered by a physician for a documented medical indication — such as symptoms of hypogonadism, infertility, or PCOS — most insurance plans provide coverage. Self-pay patients receive transparent, upfront pricing with no hidden charges.
It is worth noting that the individual testosterone test is the most affordable entry point, but a comprehensive panel provides significantly more diagnostic value. Total testosterone alone can be misleading if SHBG is abnormally high or low. Investing in a full panel from the outset often prevents the need for repeat testing and saves both time and money in the long run.
Book Your Testosterone Test at DCDC
Individual testosterone tests from AED 200. Full male hormone panels from AED 750. Morning appointments available 7 days a week at Dubai Healthcare City.
Call +971 56 403 3528 or WhatsApp to book
What Happens After Your Test: Reading Your Results
Once your testosterone blood sample has been analysed — typically within 24–48 hours at DCDC — your results will be reported with reference ranges specific to your age and sex. Understanding what these numbers mean requires context beyond simply checking whether you fall within the normal range.
Interpreting Total Testosterone
A total testosterone result below 300 ng/dL (10.4 nmol/L) on a properly timed morning sample is considered low by Endocrine Society standards. However, a single low reading is not sufficient for diagnosis — the guidelines require two separate morning measurements showing consistently low levels before hypogonadism is confirmed. This is because testosterone levels can be temporarily suppressed by illness, stress, sleep deprivation, or medication use.
When Total Testosterone Is Misleading
Total testosterone can be within the normal range while the biologically active fraction is low. This occurs when SHBG is elevated — more testosterone is bound and unavailable to tissues. Common scenarios include men over 50 (SHBG increases with age), men with liver disease or hyperthyroidism, and men taking certain medications. In these cases, free testosterone and bioavailable testosterone provide a more accurate assessment.
Understanding the Full Picture
Your doctor will interpret testosterone results alongside LH and FSH to determine whether a low testosterone level originates from the testes (primary hypogonadism, characterised by high LH and FSH) or from the pituitary gland or hypothalamus (secondary hypogonadism, characterised by low or inappropriately normal LH and FSH). This distinction is critical because it determines the cause and guides treatment. Additional tests such as prolactin, thyroid function, iron studies, and a metabolic panel may be ordered based on the clinical picture.
Managing conditions that commonly coexist with low testosterone — such as diabetes management and metabolic syndrome — can sometimes improve testosterone levels without the need for hormone replacement.
How DCDC Tests Testosterone in Dubai Healthcare City
At Doctors Clinic Diagnostic Center (DCDC), testosterone testing follows a structured clinical pathway designed to ensure accurate diagnosis and efficient follow-up. Located in Building 64 of Dubai Healthcare City, our MOHAP-licensed laboratory and specialist clinics operate under one roof.
Step 1: Consultation or Direct Testing
You can either book a GP consultation (from AED 150) to discuss your symptoms before testing, or request a testosterone panel directly as a self-pay patient. For insurance-covered testing, a physician order is typically required. Walk-ins are welcome for both consultations and blood draws.
Step 2: Morning Blood Draw
Our phlebotomy team collects your sample between 7 and 10 AM. The draw takes under five minutes and involves a standard venepuncture from the arm. If a comprehensive panel has been ordered, all tests are drawn from a single sample — no need for multiple needle sticks.
Step 3: Laboratory Analysis
Samples are processed on-site using advanced immunoassay analysers. Testosterone, free testosterone, SHBG, and gonadotropins are measured with high precision, and results are typically available within 24–48 hours.
Step 4: Results Review and Next Steps
Results are reviewed by a physician, and you can collect them via our patient portal or during a follow-up appointment. If your results are abnormal, referral to an in-house urologist or endocrinologist can be arranged — often for the same week. If a second confirmatory morning sample is needed (as required by Endocrine Society guidelines), this is scheduled promptly.
- MOHAP-licensed laboratory: Accredited testing with quality-controlled immunoassay platforms
- Morning appointments 7 days a week: Ensuring correct timing for circadian-dependent hormones
- Integrated specialist referral: Urology and endocrinology in the same building
- Insurance accepted: Direct billing with 20+ major Dubai insurers
- Fast turnaround: Most results within 24–48 hours
- Convenient DHCC location: Building 64, near Oud Metha Metro
Lifestyle Factors That Affect Your Testosterone Levels
Before considering medical intervention, it is important to recognise that lifestyle factors have a profound impact on testosterone production. In many cases — particularly when testosterone is borderline low rather than severely deficient — lifestyle modification can produce meaningful improvements.
Body Composition and Weight
Obesity is the single strongest modifiable risk factor for low testosterone. Adipose tissue contains the enzyme aromatase, which converts testosterone to oestrogen. The more body fat a man carries, the more testosterone is lost to this conversion. Studies show that losing 10–15% of body weight can increase testosterone by 50–100 ng/dL in obese men. Conversely, very low body fat (below 8%) — common in extreme endurance athletes — can also suppress testosterone through a different mechanism involving energy availability.
Exercise
Resistance training (weightlifting) is the most effective form of exercise for boosting testosterone. Compound movements such as squats, deadlifts, and bench presses that recruit large muscle groups produce the greatest hormonal response. High-intensity interval training (HIIT) also supports testosterone production. However, chronic overtraining without adequate recovery can have the opposite effect, raising cortisol and suppressing the hypothalamic-pituitary-gonadal axis.
Sleep
Testosterone is produced primarily during sleep, with peak secretion occurring during REM phases. Research published in the Journal of the American Medical Association found that one week of sleeping only 5 hours per night reduced testosterone levels in young healthy men by 10–15% — equivalent to ageing 10–15 years. Prioritising 7–9 hours of quality sleep is one of the most effective natural strategies for maintaining testosterone levels.
Stress and Cortisol
Cortisol and testosterone have an inverse relationship. Chronic psychological or physical stress elevates cortisol, which directly suppresses GnRH (gonadotropin-releasing hormone) at the hypothalamic level, reducing the downstream signal to produce testosterone. Stress management through exercise, adequate sleep, and when necessary professional support, can help restore hormonal balance.
Nutrition and Micronutrients
Several micronutrients are essential cofactors for testosterone synthesis. Zinc is required for Leydig cell function and testosterone production. Vitamin D functions as a steroid hormone precursor and is associated with testosterone levels in multiple studies — a significant concern in Dubai where vitamin D deficiency affects up to 80% of the UAE population despite abundant sunshine. Magnesium, vitamin B6, and healthy dietary fats also support testosterone production. Excessive alcohol consumption suppresses testosterone acutely and chronically.
When to See a Specialist: Beyond the Blood Test
A GP can order and interpret your testosterone test, but certain situations warrant referral to a specialist. At DCDC, our endocrinology and urology departments provide advanced evaluation and treatment for complex hormonal conditions.
Referral to a Urologist
A urologist should be involved when low testosterone is accompanied by erectile dysfunction that does not respond to first-line treatment, infertility or low sperm count requiring evaluation, suspected testicular pathology (varicocele, testicular atrophy, or masses), or when testosterone replacement therapy (TRT) is being considered. TRT requires careful monitoring of haematocrit, PSA (prostate-specific antigen), lipid profile, and liver function, and a urologist experienced in hormone management ensures safe, optimised therapy.
Referral to an Endocrinologist
An endocrinologist is appropriate when laboratory findings suggest secondary hypogonadism (low testosterone with low or normal LH and FSH), which may indicate pituitary pathology — including pituitary adenomas that produce excess prolactin. Endocrinology referral is also indicated when testosterone deficiency coexists with other endocrine disorders such as thyroid disease, adrenal insufficiency, or diabetes, or when the clinical picture is complex and does not respond to initial management.
When Lifestyle Optimisation Is Enough
Not every man with borderline-low testosterone needs medical treatment. When levels are between 250 and 350 ng/dL and symptoms are mild, a focused programme of weight management, resistance exercise, sleep optimisation, stress reduction, and nutritional supplementation (zinc, vitamin D, magnesium) can often raise testosterone into the symptomatic improvement range within 3–6 months. Your GP can retest after this period to assess progress.
Get Your Testosterone Levels Checked Today
Testosterone tests from AED 200. Full male hormone panels from AED 750. Results in 24–48 hours with same-week specialist referral if needed.
WhatsApp +971 56 403 3528 for morning appointments
Kaugnay na Serbisyo sa DCDC
Dalubhasang pangangalaga at advanced diagnostics sa Dubai Healthcare City
Hormone Testing
Comprehensive male and female hormone panels with results in 24-48 hours
Mag-book ng AppointmentBlood Tests
Full blood work including CBC, metabolic panel, and specialized markers
Mag-book ng AppointmentHealth Checkup
Annual wellness screening with hormone panel add-on option
Mag-book ng AppointmentMga Madalas Itanong
Final Thoughts
Testosterone testing is a straightforward blood test that can provide critical answers for men and women experiencing symptoms of hormonal imbalance. Whether you are dealing with unexplained fatigue, changes in body composition, low libido, mood disturbances, or fertility difficulties, a properly timed morning testosterone test is the essential first step toward diagnosis and treatment. Understanding your levels — and how they relate to your age, symptoms, and overall health — empowers you and your physician to make informed decisions.
At DCDC in Dubai Healthcare City, we offer individual testosterone tests from AED 200 and comprehensive male hormone panels from AED 750, with morning appointments available seven days a week and results typically within 24–48 hours. Our integrated approach means your results are reviewed by a GP and, when needed, referred to an in-house urologist or endocrinologist — often within the same week. Book your test today by calling +971 56 403 3528 or send us a WhatsApp message.
Mga Sanggunian at Reperensya
Ang artikulong ito ay sinuri ng aming medikal na team at tumutukoy sa mga sumusunod na sanggunian:
- Endocrine Society - Testosterone Therapy in Men with Hypogonadism: An Endocrine Society Clinical Practice Guideline (2018)
- American Urological Association - Evaluation and Management of Testosterone Deficiency (2018)
- Leproult R, Van Cauter E - Effect of 1 Week of Sleep Restriction on Testosterone Levels in Young Healthy Men, JAMA (2011)
- Cleveland Clinic - Low Testosterone (Male Hypogonadism): Symptoms, Causes & Treatment
- Mayo Clinic - Testosterone Therapy: Potential Benefits and Risks
- Travison TG et al. - A Population-Level Decline in Serum Testosterone Levels in American Men, Journal of Clinical Endocrinology & Metabolism (2007)
- Rotterdam ESHRE/ASRM-Sponsored PCOS Consensus Workshop Group - Revised 2003 Consensus on Diagnostic Criteria for PCOS
Ang medikal na nilalaman sa site na ito ay sinusuri ng mga DHA-licensed na manggagamot. Tingnan ang aming patakarang editorial para sa higit pang impormasyon.
Related Articles
Hormone Test Dubai: Types, Cost & Guide (2026)
Blood Test Dubai: Types, Cost & Fasting Guide (2026)

Health Checkup Cost in Dubai: AED 800-6,000 by Package (2026)

Hair Loss Treatment Dubai: Costs & Options (2026)

Annual Health Checkup: Tests You Need by Age (2026)
blogPage.moreFromCategory
Ankle Sprain Dubai: Treatment & Recovery (2026)
Basahin Pa
Urine Test Dubai: Types, Cost & Guide (2026)
Basahin Pa
Thyroid Problems Symptoms Dubai (2026)
Basahin Pa
Newborn Screening Tests Dubai: Full Guide (2026)
Basahin Pa
Sore Throat Dubai: Causes & Treatment (2026)
Basahin Pa
Torn Meniscus Dubai: Signs & Treatment (2026)
Basahin Pa© 2026 Doctors Clinic Diagnostic Center (DCDC), Dubai Healthcare City. Originally published at https://doctorsclinicdubai.ae/blog/testosterone-test-dubai-guide. All rights reserved. Unauthorized reproduction is prohibited.