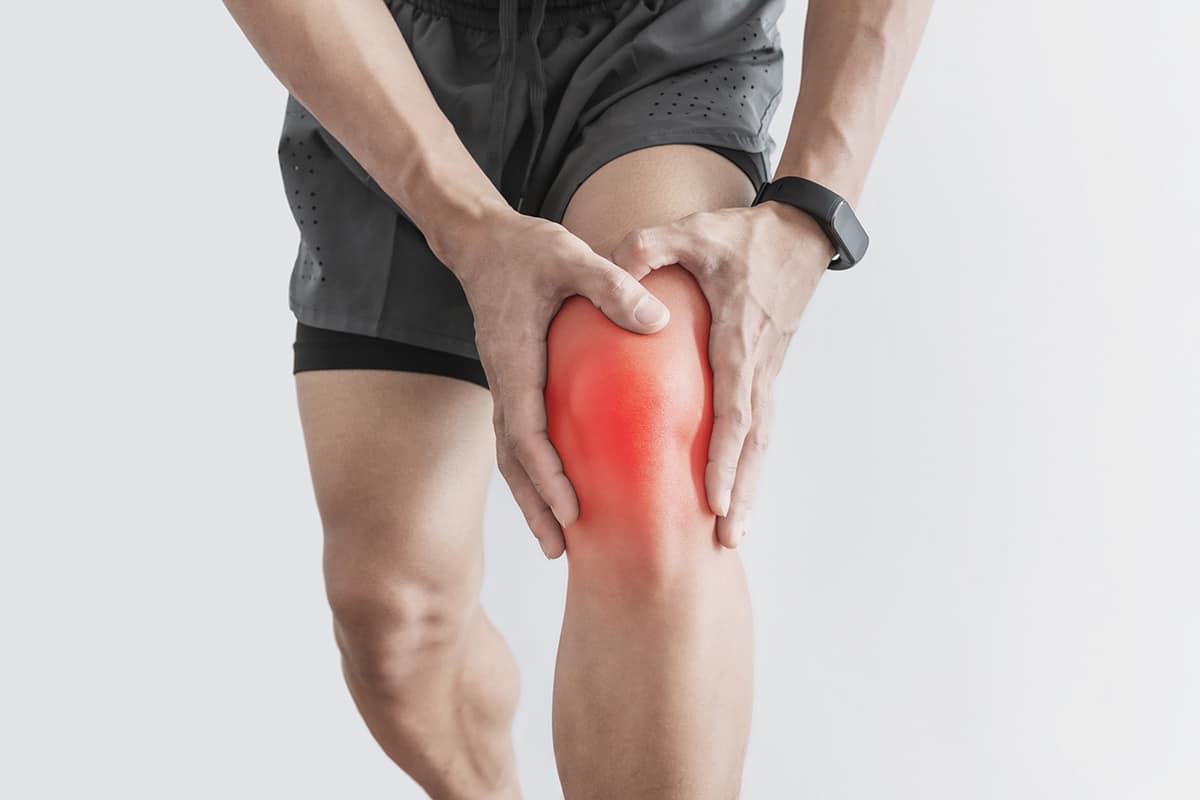
نکات کلیدی
- Exercise is the single most effective non-surgical treatment for knee osteoarthritis -- stronger evidence than any medication
- Physiotherapy cannot reverse cartilage loss or structural joint damage, but it can significantly reduce pain and improve function
- Strengthening the muscles around an arthritic joint reduces load on the joint itself, slowing progression and reducing pain
- Osteoarthritis (wear-and-tear) and rheumatoid arthritis (autoimmune) require fundamentally different medical management
- Weight loss of just 5-10% of body weight can reduce knee OA pain by 50% -- the most impactful lifestyle change
- Joint replacement should be considered when pain significantly impacts quality of life despite consistent conservative treatment
- Low-impact exercise (swimming, cycling, walking) is safe for arthritic joints and does not accelerate cartilage loss
- The belief that exercise wears out arthritic joints is a myth that leads to harmful deconditioning
You have been told you have arthritis and that it will only get worse. Maybe you have seen the X-ray showing bone-on-bone changes and assumed there is nothing to do except wait for a joint replacement. This is one of the most damaging misconceptions in musculoskeletal medicine. At our physiotherapy clinic in Dubai Healthcare City, we help patients with arthritis reduce pain, improve mobility, and often delay or avoid surgery entirely -- but we are also honest about what physiotherapy cannot change.
Arthritis is the leading cause of disability worldwide, affecting over 500 million people. In Dubai's population, osteoarthritis of the knee and hip is particularly common, driven by rising obesity rates, sedentary lifestyles, and an ageing population. This guide covers what the evidence actually says about exercise and physiotherapy for arthritis, without overselling or underselling what it can achieve.
What Is the Difference Between Osteoarthritis and Rheumatoid Arthritis?
These two conditions share the word "arthritis" but are fundamentally different diseases with different causes, treatment, and prognosis. Many patients we see are unsure which type they have, which matters because the management approach differs significantly.
| Feature | Osteoarthritis (OA) | Rheumatoid Arthritis (RA) |
|---|---|---|
| Cause | Cartilage degeneration and joint changes over time | Autoimmune attack on the joint lining (synovium) |
| Typical onset | Gradual, usually after age 45 | Can start at any age, often 30-50 |
| Joints affected | Knees, hips, hands (DIP joints), spine | Small joints of hands and feet (MCP, PIP joints) symmetrically |
| Morning stiffness | Less than 30 minutes | More than 1 hour |
| Inflammation | Mild, mechanical | Significant, systemic |
| Blood tests | Usually normal (CRP, ESR may be mildly elevated) | Elevated CRP, ESR, positive RF and anti-CCP antibodies |
| Medical treatment | Pain management, exercise, weight loss, injections | Disease-modifying drugs (DMARDs), biologics, steroids |
| Physiotherapy role | Central to management -- first-line treatment | Important adjunct alongside medical management |
This table covers the most common differences. Some patients have both OA and RA, and other forms of arthritis (gout, psoriatic) have distinct features.
Why Is Exercise Better Than Medication for Knee Osteoarthritis?
This is not an exaggeration or marketing claim. Multiple high-quality systematic reviews, including Cochrane reviews and guidelines from the American College of Rheumatology, consistently rank exercise as the most effective non-surgical treatment for knee OA -- superior to paracetamol, NSAIDs, and supplements. A landmark 2015 BMJ meta-analysis found that exercise therapy produced pain reductions equivalent to NSAIDs but with additional benefits in function, no side effects, and effects that persist as long as the exercise continues.
How does this work? Exercise strengthens the muscles around the joint, reducing the load on the damaged cartilage. It improves joint nutrition (cartilage gets its nutrients from joint fluid, which is pumped by movement). It reduces inflammation, improves proprioception (joint awareness), and has potent effects on pain perception through central nervous system mechanisms. The key is that the right type and dose of exercise matters.
What Types of Exercise Help Arthritis?
An effective arthritis exercise programme includes three components: strengthening, aerobic conditioning, and flexibility. Each addresses a different aspect of the condition. Your physiotherapist will build a programme based on which joints are affected, your current fitness level, and your goals. For related information, see our guide on Runner's Knee: Physio Treatment & Recovery.
Strengthening Exercises
- Quadriceps strengthening (for knee OA): Straight leg raises, wall sits, mini squats, leg press. Weak quadriceps are the strongest modifiable risk factor for knee OA progression. Aim for 3 sets of 10-15 repetitions, 3 times per week
- Hip strengthening (for hip and knee OA): Side-lying hip abduction, clamshells, bridges, step-ups. Strong hip muscles reduce abnormal knee loading
- Grip strengthening (for hand OA): Putty exercises, gentle gripping activities. Maintaining hand strength preserves independence
- Core strengthening (for spinal OA): Modified planks, bird-dogs, pelvic tilts. Supports the spine and reduces pain
Aerobic Exercise
- Walking: 30 minutes, 5 times per week. The most accessible and well-studied exercise for OA. Use supportive footwear on flat surfaces
- Swimming and water aerobics: Buoyancy reduces joint load by 50-75%. Excellent for people with severe OA or obesity who find land-based exercise painful
- Cycling (stationary or outdoor): Low impact, builds quadriceps strength, and provides aerobic benefit. Adjust seat height to minimise knee stress
- Elliptical trainer: Low impact with full-body engagement. Good gym-based alternative to running
Flexibility and Range of Motion
- Gentle stretching of muscles around affected joints -- held for 30 seconds, repeated 3 times
- Range-of-motion exercises to maintain full joint movement -- especially important for hips and knees
- Yoga and tai chi have strong evidence for arthritis symptom management and balance improvement
What Joint Protection Strategies Help Arthritis?
Joint protection is about reducing unnecessary stress on arthritic joints during daily activities without avoiding movement entirely. These are practical strategies your physiotherapist will teach alongside your exercise programme.
- Pacing activities: Break prolonged standing, walking, or repetitive tasks into smaller chunks with rest periods
- Using larger joints: Carry bags with your forearms rather than your fingers. Push doors with your body rather than your hands
- Assistive devices: A walking stick (held on the opposite side to the affected knee) reduces knee joint loading by 20-30%
- Ergonomic modifications: Raised toilet seats, chair height adjustments, jar openers, and lever-style door handles reduce strain on arthritic joints
- Appropriate footwear: Cushioned, supportive shoes. Avoid high heels. For medial knee OA, lateral wedge insoles may help distribute load
How Much Does Weight Loss Help Arthritis?
Weight management is perhaps the most impactful intervention for knee and hip OA, yet it is often underemphasised. Every 1kg of body weight lost reduces the load on the knee by 4kg during walking. The IDEA trial (2013) demonstrated that losing just 10% of body weight reduced knee pain by 50% and improved function by 28%. For a person weighing 90kg, this means losing 9kg can halve their knee pain -- a result that no medication can match without side effects.
Combining weight loss with exercise produces better results than either alone. This is why a comprehensive arthritis management plan at DCDC often includes coordination with our joint pain management team and nutritional guidance.
What Can Physiotherapy NOT Do for Arthritis?
Being honest about limitations builds trust and helps patients set realistic expectations. Physiotherapy cannot reverse structural damage that has already occurred. Here is what it genuinely cannot achieve: You may also find our Scoliosis Physiotherapy: Exercises & Treatment helpful.
- Regrow lost cartilage: Once cartilage is worn away, it does not regenerate. Exercise cannot rebuild it
- Remove bone spurs (osteophytes): These structural changes are permanent without surgery
- Cure rheumatoid arthritis: RA requires disease-modifying medication. Physiotherapy manages symptoms alongside medical treatment
- Reverse joint deformity: Advanced joint changes (knock knees, bow legs from OA) are structural
- Eliminate all pain in advanced OA: When bone grinds on bone with every step, exercise reduces but may not eliminate pain
What physiotherapy can do is reduce pain, improve function, slow progression, delay joint replacement by years, improve post-surgical outcomes, and maintain independence. These are not small achievements -- for many patients, a structured exercise programme is the difference between an active life and progressive disability.
When Does Joint Replacement Become Necessary?
Joint replacement (arthroplasty) is one of the most successful surgeries in medicine, with 90-95% of patients experiencing significant pain relief and improved function. However, timing matters. There is no X-ray finding that determines when surgery is needed -- the decision is based on the impact on your quality of life despite having tried appropriate conservative management.
- Pain that significantly affects sleep, walking, and daily activities despite 3-6 months of consistent exercise and weight management
- Inability to walk reasonable distances (less than 500 metres without stopping)
- Pain requiring regular strong analgesics to get through the day
- Significant joint deformity affecting alignment and gait
- Quality of life has deteriorated to the point where you are avoiding activities you value
If joint replacement is being considered, pre-surgical physiotherapy ("prehabilitation") improves post-surgical outcomes. Patients who enter surgery stronger and with better mobility recover faster and achieve better long-term results. Our orthopaedic specialists at DCDC can assess whether you are at the right stage for this discussion.
Managing Arthritis Pain? Get an Expert Assessment
Whether you are newly diagnosed or have been managing arthritis for years, our physiotherapy team at DCDC Dubai Healthcare City can build an exercise programme tailored to your joints, your fitness level, and your goals. Exercise is not optional for arthritis -- it is the most effective treatment available.
Book a Physiotherapy Consultation
خدمات مرتبط در DCDC
مراقبت تخصصی و تشخیص پیشرفته در شهر بهداشت دبی
سؤالات متداول
Final Thoughts
Arthritis is not a death sentence for your active life. The evidence is overwhelming that exercise is the most effective treatment for osteoarthritis, and structured physiotherapy provides the guidance to exercise safely and effectively. At the same time, being honest about what physiotherapy cannot do -- reverse cartilage loss, cure RA, or eliminate all pain in advanced disease -- helps you make informed decisions about your management.
If you have arthritis and are not currently exercising, the single most important step you can take is to start. Our physiotherapy team at DCDC Dubai Healthcare City will ensure you start at the right level, progress safely, and build a sustainable programme that fits your life. The best time to start was when you were diagnosed. The second-best time is now.
منابع و مراجع
این مقاله توسط تیم پزشکی ما بررسی شده و به منابع زیر ارجاع میدهد:
- BMJ - Exercise Therapy for Knee Osteoarthritis Meta-Analysis (2015)
- Cochrane Review - Exercise for Osteoarthritis of the Knee (2022)
- American College of Rheumatology - OA Management Guidelines (2020)
- Arthritis & Rheumatology - Walking and Knee OA Progression (2022)
- World Health Organization - Musculoskeletal Health (2023)
- Dubai Health Authority - Chronic Disease Management Standards
محتوای پزشکی این سایت توسط پزشکان دارای مجوز DHA بررسی میشود. مشاهده سیاست تحریریه برای اطلاعات بیشتر.
Related Articles

Complete Guide to Physiotherapy in Dubai: Types, Costs & What to Expect
Frozen Shoulder Treatment: A Physiotherapy Approach

How Many Physiotherapy Sessions Do You Need?

Physiotherapy Cost in Dubai 2026: Pricing & Packages
blogPage.moreFromCategory
PRP vs Cortisone Dubai: Which Injection? (2026)
بیشتر بخوانید
PRP Injection for Joints Dubai: From AED 1,500 (2026)
بیشتر بخوانید
Physiotherapy Dubai: Types, Cost & Guide (2026)
بیشتر بخوانید
Physiotherapy Cost Dubai: AED 250–500/Session (2026)
بیشتر بخوانید
Carpal Tunnel: Non-Surgical Treatment Dubai (2026)
بیشتر بخوانید
Pediatric Physiotherapy Dubai: When Kids Need It (2026)
بیشتر بخوانید© 2026 Doctors Clinic Diagnostic Center (DCDC), Dubai Healthcare City. Originally published at https://doctorsclinicdubai.ae/blog/arthritis-physiotherapy-management. All rights reserved. Unauthorized reproduction is prohibited.